The National Comprehensive Cancer Network issued a guidance for COVID-19 vaccinations in people with cancer.
The NCCN COVID-19 Committee’s recommendations state that all people currently in active cancer treatment should get the vaccine, with some advice to consider regarding immunosuppression and timing. The full document can be found here.
The NCCN COVID-19 Vaccine Committee includes hematology and oncology experts with particular expertise in infectious diseases, vaccine development and delivery, medical ethics, and health information technology.
These recommendations can help cancer care providers make informed decisions on how to protect their patients from the ongoing COVID-19 pandemic, based on available evidence plus expert consensus.
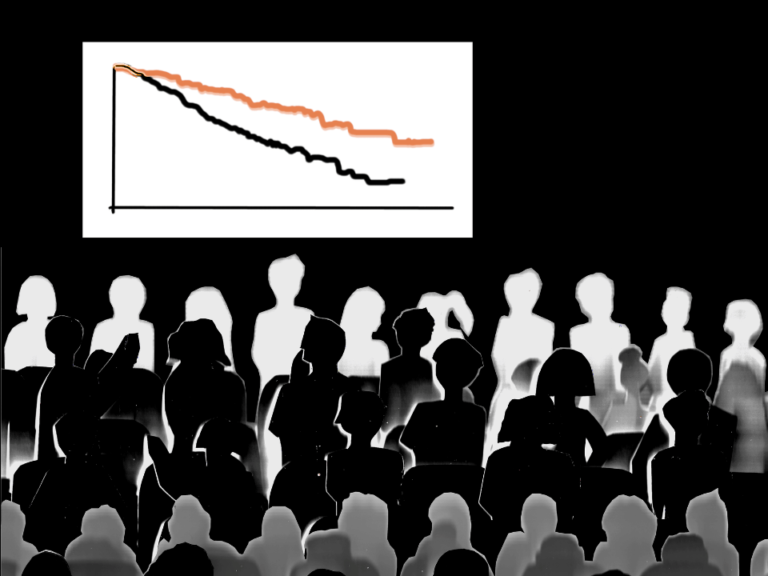
“Our number one goal is helping to get the vaccine to as many people as we can,” NCCN COVID-19 Vaccine Committee Co-leader Steve Pergam said in a statement. “That means following existing national and regional directions for prioritizing people who are more likely to face death or severe illness from COVID 19. The evidence we have shows that people receiving active cancer treatment are at greater risk for worse outcomes from COVID-19, particularly if they are older and have additional comorbidities, like immunosuppression.”
Pergam is also associate professor of the Vaccine and Infectious Disease Division at Fred Hutchinson Cancer Research Center and Infection Prevention Director at Seattle Cancer Care Alliance.
“Too many caveats can lead to confusion,” committee co-leader Lindsey Baden, associate professor of medicine, infectious disease of Brigham and Women’s Hospital and Dana-Farber Cancer Institute, said in a statement. “If strong new evidence comes out to support prioritizing certain groups over others, we can always adjust. This is intended to be a living document that is constantly evolving—it will be updated rapidly whenever new data comes out, as well as any potential new vaccines that may get approved in the future.”
The guidance statement from NCCN builds off of existing understanding and guidelines for the flu vaccine during active cancer treatment—such as those in the NCCN Clinical Practice Guidelines in Oncology for Prevention and Treatment of Cancer-Related Infections.
“One of our primary goals is reducing morbidity and mortality,” Sirisha Narayana, associate professor of medicine and chair of the UCSF Ethics Committee at UCSF Health, said in a statement. “We also have to take social determinants of health into account and make special efforts for people in high-risk communities.”
The guidance acknowledges that although these vaccines have been shown to be safe in general populations, their effectiveness among cancer and transplant patients is not precisely known at present.
Available data from vaccine trials have demonstrated that vaccines decrease the incidence of COVID-19 disease and complications, but it is unclear if these vaccines prevent infection and subsequent transmission.
Therefore, everyone should continue to wear masks, avoid large gatherings, and follow other recommendations for preventing COVID-19 acquisition and transmission, even after vaccination. The committee feels strongly that caregivers and other members of the same household should also be encouraged to get the vaccine as soon they are considered eligible where they live.
The committee also addressed:
How to prioritize patients in the event of limited supplies and staff capacity.
How to recommend appropriate scheduling based around immunosuppressive therapy.
How to prepare for possible medication interactions or adverse events.
How to account for societal inequities and prioritize at-risk communities.
How to communicate with patients and caregivers, particularly non-English speakers.
The balance of vaccination efforts between the cancer center and community settings.
The panel will continue to meet regularly in order to refine the recommendations for these and other issues, as they come up. Any open questions can also serve as a guide for areas where new research is most needed.