Emil J Freireich was a big man in stature, with a booming voice. He was one of the last of the 60 original members of the American Society of Clinical Oncology.


Photo courtesy of MD Anderson Cancer Center
He would go on to impact the profession for nearly seven decades. In the process, he trained hundreds of oncologists and influenced thousands.
He was friendly, often confrontational, but always supportive of young talent. Perhaps it came from his childhood in Chicago. He lived in poverty. He went to the University of Illinois by train, and personally persuaded someone in the admissions office to admit him. He worked as a waiter in a sorority to pay the tuition.
He went on to the University of Illinois for medical school and did residency at Cook County Hospital. He was outraged that they gave up on the cancer patients and put them in “the corner room” to die.
In the 1950s, this fellow from humble beginnings would work with several men who would become giants of oncology: Gordon Zubrod, James Holland and Emil Frei. Together, they made up a large part of the National Cancer Institute Clinical Program.
People called him “J” to distinguish him from the other fellow who by coincidence had an almost identical name.
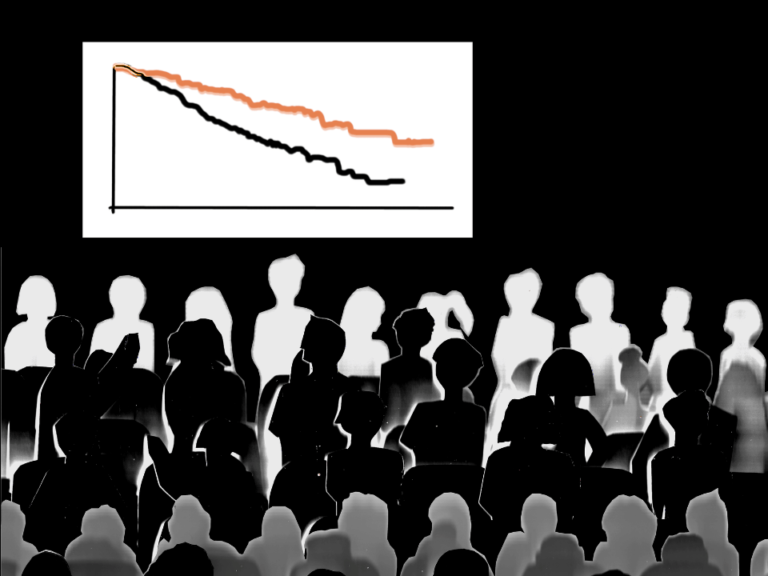
J would become one of the originators of the concept of combination chemotherapy, platelet transfusions, and establish many of the rules of cancer treatment used to this day. Later in life, he would give a talk entitled “How we cured childhood leukemia.”
There are very few of us in oncology who could give a talk entitled “How we cured anything.”
J was always controversial. I got to know him when he was sent on sabbatical to the NCI from MD Anderson to write a paper on the training of young oncologists. I learned that he was quick to tell you he disagreed with you.
Even though he disagreed with a young oncologist, he would still support them and even occasionally point out a fact that suggested his point of view was wrong, sometimes asking, “Why didn’t you see that?”
In a long lunchtime conversation, he and I disagreed once on the value of phase III clinical trials. J felt that it is obvious if a drug works, and phase III clinical trials are an attempt to market something that does not work.
He rather loudly asked me if there had ever been a phase III trial of cisplatin in testicular cancer. I said no.
Realizing others in the lunchroom were listening and he had an audience, he came up with one of his famous lines: Phase III studies are only for product promotion, and the only reasonable phase III trial was a comparison of Coke versus Pepsi.
He was fair and open-minded and ahead of his time. He trained and mentored people from many backgrounds and multiple countries. It would not unusual for Freireich to have someone from Israel working with someone from Lebanon.
He was quick to point out that no race and no country has a monopoly on good talent.
Recently, I was talking to another of the greats of oncology and the subject of J came up. We both remembered the ASCO meeting of 2000 in New Orleans.
The president’s reception was in the then relatively new World War II Museum. Emil Frei was then wheelchair-bound due to Parkinson’s.
Freireich pushed Frei around in the wheelchair all night. To those of us who appreciate the field, there was something special about two men who had done so much for oncology and really liked and admired each other.
The authoer is Bloomberg Distinguished Professor of Oncology and Epidemiology, Johns Hopkins University
Co-editor, Cancer History Project