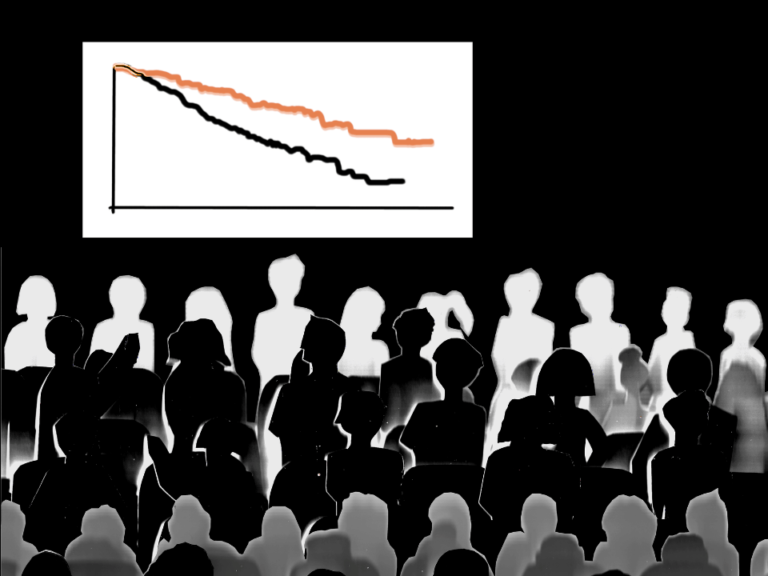
Oct. 25, we heard more about President Trump’s plan to save health care dollars through a variety of Medicare pilot programs and index pricing.
One of the proposed strategies seeks to lower Medicare Part B drug prices by indexing them to the much lower prices paid by 16 countries (referred to as the International Pricing Index, or IPI). This model would be piloted in randomly selected geographic areas and would be mandatory for providers. Essentially, the price of some Part B drugs, including cancer drugs and biologics, would gradually shift to international prices
Accompanying the IPI model, a second strategy dismantles the current buy-and-bill system, where providers purchase Part B drugs, add a handling fee, and bill their patients. In its place, private sector vendors who have contracted with the Centers of Medicare and Medicaid Services will procure drugs and distribute them to providers (who will receive a set handling fee).
CMS will then pay these vendors based on the IPI price. The proposal anticipates that these private sector vendors would drive a hard bargain with manufacturers, and compete for providers’ business.
The success of this plan depends on drug companies agreeing to sell their products at lower prices. If they aren’t willing to make these concessions, the private sector vendors may simply choose not to purchase them, resulting in patients being deprived of access to these drugs.
Since Part B coverage extends to whatever is “reasonable and necessary for the diagnosis and treatment of illness and injury,” CMS cannot refuse reimbursement based on a belief that the price for a treatment is too high. That said, however, the legal and administrative actions that could arise from disputes around these issues are mindboggling. More wheel-spinning at CMS helps no one and wastes more resources.
Two additional risks have me quite concerned:
One relates to the chaos and confusion that could arise from the introduction of “private sector vendors” to the drug distribution chain. Jeopardizing cancer patient access to life-saving treatments is simply unacceptable.
A second, longer-term risk is that pharmaceutical manufacturers take significant revenue hits that stifle their commitment to research and innovation. We all depend on drug discovery to drive better therapies and find cures. This is where hope lives.
Let’s think about healthcare as a true partnership between patients and providers. Instead of delivering healthcare ‘to patients,’ treatment plans should be determined and provided ‘with patients.’
When all is said and done, the Trump plan represents merely an advance notice of proposed rulemaking. It kicks off a long regulatory process that could last months if not years. Normally, a pre-rule precedes a proposed rule and then becomes a final rule before any changes are implemented, and the government must accept and respond to comments from the public at each stage.
To ivory tower bureaucrats and politicians, spending fewer healthcare resources may seem like the impossible dream. To those of us in the trenches who witness the delivery of healthcare services to patients every day, there are some very simple ways to make a sizable dent in spending and improve the delivery of value. Mostly, this is not about the price of drugs.
Six years ago, ASCO’s expert panel for the Choosing Wisely campaign identified use of chemotherapy in patients for whom no proven benefit existed as one of the most widespread, wasteful, and unnecessary practices in oncology.
Also, consider these studies:
A recent study published in BMJ found the use of chemotherapy in terminally ill cancer patients in the last months of life to be associated with an increased risk of undergoing CPR, mechanical ventilation or both and of dying in an intensive care unit. BMJ. 2014 Mar 4;348:g1219. doi: 10.1136/bmj.g1219.
A study in JAMA reported that among family members of older patients with fee-for-service Medicare who died of lung or colorectal cancer, earlier hospice enrollment, avoidance of ICU admissions within 30 days of death, and death occurring outside the hospital were associated with perceptions of better end-of-life care. JAMA. 2016 Jan 19;315(3):284-92. doi: 10.1001/jama.2015.18604
Despite widespread awareness of this issue among cancer care providers, there continues to be vast overuse of chemotherapy among metastatic patients, driving excessive medical bills and causing physical and emotional distress among patients and families.
What’s the swift and obvious answer?
Have the tough conversations that can uncover patients’ quality of life preferences and priorities. Urge patients and families to tell their providers what really matters during and after cancer treatment—and document these conversations with Advance Directives.
Let’s think about healthcare as a true partnership between patients and providers. Instead of delivering healthcare “to patients,” treatment plans should be determined and provided “with patients.”
Switching “to” to “with” has the potential to drive enormous savings, because patients will likely want quality of life over quantity of life.
I know that I will.