European Commission has approved an expanded indication for XGEVA (denosumab) for the prevention of skeletal-related events in adults with advanced malignancies involving bone.
The indication now covers patients with bone metastases from solid tumors and those with multiple myeloma. The approval is based on data from the phase III ‘482 study, the largest international trial ever conducted for the prevention of skeletal-related events in multiple myeloma patients.
XGEVA is sponsored by Amgen Inc.
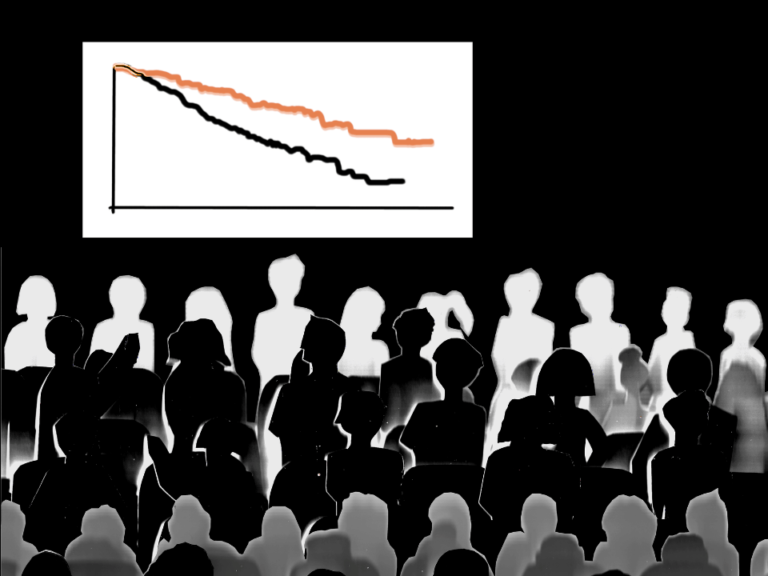
In the ‘482 study, XGEVA met the primary endpoint, demonstrating non-inferiority to zoledronic acid in delaying the time to first on-study skeletal-related event in patients with multiple myeloma (HR=0.98, 95 percent CI: 0.85-1.14).
The median time to first on-study skeletal-related event was 22.8 months for XGEVA and 24.0 months for zoledronic acid. The safety profile was consistent with known adverse events of XGEVA.
XGEVA is the first fully human monoclonal antibody that binds to and neutralizes RANK ligand, a protein essential for the formation, function and survival of osteoclasts, thereby inhibiting osteoclast-mediated bone destruction.
On Jan. 5, FDA approved the supplemental Biologics License Application for XGEVA to expand the currently approved indication for the prevention of skeletal-related events in patients with bone metastases from solid tumors to include patients with multiple myeloma.
Additional regulatory applications for XGEVA for the prevention of skeletal-related events in patients with multiple myeloma are underway and have been submitted to health authorities worldwide.
The ‘482 study was an international, phase III, randomized, double-blind, multicenter trial of XGEVA compared with zoledronic acid in the prevention of skeletal-related events in adult patients with newly diagnosed multiple myeloma and bone disease.
In the study, a total of 1,718 patients (859 on each arm) were randomized to receive either subcutaneous XGEVA 120 mg and intravenous placebo every four weeks, or intravenous zoledronic acid 4 mg (adjusted for renal function at baseline) and subcutaneous placebo every four weeks, plus investigators’ choice first-line antimyeloma therapy.
Skeletal surveys using conventional radiography were obtained every 12 to 24 weeks per protocol. The primary endpoint of the study was non-inferiority of XGEVA versus zoledronic acid with respect to time to first on-study skeletal-related event (pathologic fracture, radiation to bone, surgery to bone or spinal cord compression).
Secondary endpoints included superiority of XGEVA versus zoledronic acid with respect to time to first on-study skeletal-related event and first-and-subsequent on-study skeletal-related event and evaluation of overall survival.
Progression-free survival was a prespecified, exploratory endpoint and was not powered for statistical significance. The secondary endpoints, delaying time to first skeletal-related event and delaying time to first-and-subsequent skeletal-related events, did not demonstrate superiority.
Overall survival was comparable between XGEVA and zoledronic acid, with a hazard ratio of 0.90 (95 percent CI: 0.70, 1.16). Median progression-free survival was 46.1 months (95 percent CI: 34.3 months, not estimable, n=219) for XGEVA and 35.4 months (95 percent CI: 30.2 months, NE, n=260) for zoledronic acid.
The safety and tolerability of XGEVA were also compared with zoledronic acid. The safety profile was consistent with known adverse events of XGEVA. The most common adverse reactions (greater than or equal to 10 percent) were diarrhea, musculoskeletal pain, hypocalcaemia, and dyspnea.