FDA has approved Retevmo (selpercatinib) capsules to treat non-small cell lung cancer, medullary thyroid cancer and other types of thyroid cancers in patients whose tumors have an alteration in a specific gene (RET).
Eli Lilly & Co. sponsors Retevmo.
Retevmo, a kinase inhibitor, is the first therapy approved specifically for cancer patients with the RET gene alterations. Specifically, the cancers that Retevmo is approved to treat include:
Non-small cell lung cancer that has spread in adults,
Advanced medullary thyroid cancer or MTC that has spread, in patients 12 and older who require systemic therapy (a treatment option that spreads across the entire body, is not targeted), and
Advanced RET fusion-positive thyroid cancer in those age 12 and older that requires systemic therapy that has stopped responding to radioactive iodine therapy or is not appropriate for radioactive iodine therapy.
Retevmo was approved by FDA based on the results of a clinical trial involving patients with each of the three types of tumors.
Patients received 160 mg Retevmo orally twice daily until disease progression or unacceptable toxicity. Major efficacy outcome measures were overall response rate and duration of response.
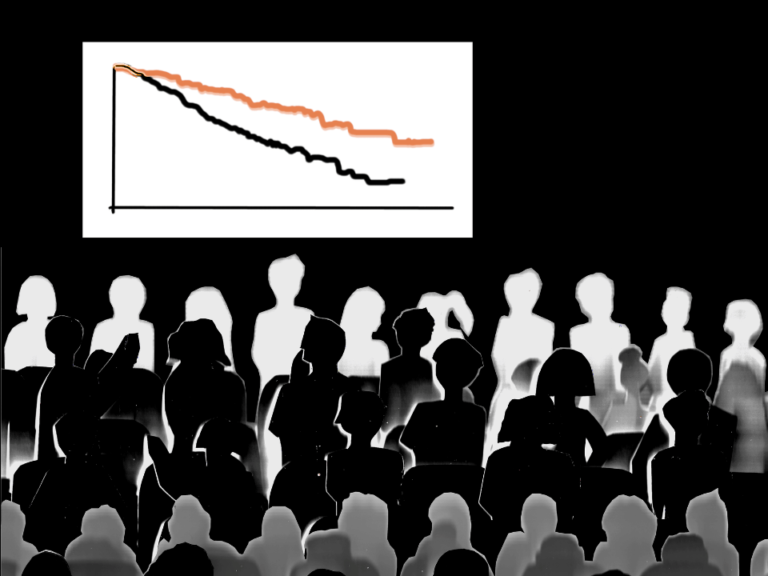
Efficacy for NSCLC was evaluated in 105 adult patients with RET fusion-positive NSCLC who were previously treated with platinum chemotherapy. The ORR for the 105 patients was 64%. For 81% of patients who had a response, their response lasted at least six months. Efficacy was also evaluated in 39 patients with RET fusion-positive NSCLC who had never undergone treatment. The ORR for these patients was 84%. For 58% of patients who had a response, their response lasted at least six months.
Efficacy for MTC in adults and pediatric patients was evaluated in those 12 and older with RET-mutant MTC. The study enrolled 143 patients with advanced or metastatic RET-mutant MTC who had been previously treated with cabozantinib, vandetanib or both, and patients with advanced or metastatic RET-mutant MTC who had not received prior treatment with cabozantinib or vandetanib. The ORR for the 55 previously treated patients was 69%.
For 76% of patients who had a response, their response lasted at least six months. Efficacy was also evaluated in 88 patients who had not been previously treated with an approved therapy for MTC. The ORR for these patients was 73%. For 61% of patients who had a response, their response lasted at least six months.
Efficacy for RET fusion-positive thyroid cancer was evaluated in adults and pediatric patients 12 years and older. The study enrolled 19 patients with RET fusion-positive thyroid cancer who were radioactive iodine-refractory and had received another prior systemic treatment, and eight patients with RET fusion-positive thyroid cancer who were RAI-refractory and had not received any additional therapy.
The ORR for the 19 previously treated patients was 79%. For 87% of patients who had a response, their response lasted at least six months. Efficacy was also evaluated in eight patients who had not received therapy other than RAI. The ORR for these patients was 100%. For 75% of patients who had a response to the treatment, their response lasted at least six months.