This story is part of The Cancer Letter’s ongoing coverage of COVID-19’s impact on oncology. A full directory of our coverage is available here.
In spite of disruptions caused by the coronavirus pandemic, NCI continues to review grants, disburse funds, and support extramural research, said NCI Director Ned Sharpless.


“I really won’t sugarcoat our present circumstances. This epidemic is bad, and it’s going to continue to be bad for a while, especially the next few weeks,” Sharpless said April 9 in an emergency virtual meeting of the NCI Board of Scientific Advisors and the National Cancer Advisory Board. “We have suspended lab operations on campus and we have stopped all non-essential activities.
“But I want to reiterate right now, from an extramural funding point of view, we are fully operational. But, no doubt, things have gotten more complicated, and we have received many, many questions from our investigators about grants, lab suspensions, and what this all means for them.
“When we do reach uniform agreement about these funding policies, the NCI is fully committed to disseminating that information as quickly as possible through blogs, our website, Twitter streams, etc.”
Thus far, two lessons for U.S. health care and oncology can be derived:
“We’ve shown that, in a meaningful way, we can take care of patients via telehealth, and I predict cancer patients are going to like this in the future,” Sharpless said. “Another area where I’ve seen a real example of something that, I think, will last after the pandemic, for the good, is the fact that the government can, when it needs to, move really quickly.
“We have been involved in complex multi-agency endeavors, but we’ve been able to really cut through a lot of the process and the usual steps to launch large, innovative, complex research efforts in a matter of days.”
The institute, with its research capabilities, has a moral obligation to be involved in the U.S. national response to the pandemic, Sharpless said.
“NCI has a long and storied history of intramural virology research, from Doug Lowy and John Schiller and Harold Varmus, to Bob Gallo, to Sam Broder—pathbreaking, groundbreaking work on HPV and HIV and RNA tumor viruses—and to not use the virology expertise at the NCI during the current pandemic would seem to be a missed opportunity,” Sharpless said.
NCI is finalizing plans to use its clinical trials networks to administer a compassionate use protocol for distribution of tocilizumab, a drug that blocks the inflammatory protein IL-6. Under the institute’s protocol, the drug will be made available to cancer patients at institutions that are not participating in Genentech’s phase III trial of the drug (The Cancer Letter, April 10, 2020).
Other updates at NCI include:
Enrollment of the first patient in a CD33 CAR T trial, a collaboration between the institute and the Children’s Hospital of Philadelphia; and
Appointment of Dan Gallahan as director of the Division of Cancer Biology.
On March 27, Congress passed a $2 trillion coronavirus relief package, the Coronavirus Aid, Relief and Economic Security (CARES) Act. The bill appropriates pandemic response funds in the following amounts: $4.3 billion for CDC, $945.4 million for NIH, $80 million for FDA, and $200 million for CMS (The Cancer Letter, March 27, 2020).
“The Congress has done some stuff for coronavirus,” Sharpless said. “Most probably relevant for the NIH is phase 3, the CARES Act, which provided significant new money for the NIH as well as the FDA and CDC, and it also—an issue I’m sure very important to many of the board members—provided significant funding for hospitals, given the massive drop in revenues some hospitals are seeing with the cessation of elective surgeries and that type of issue.”
Normalcy will return, Sharpless assured the advisory boards.
“I’m here to tell you we’ll get through this,” he said. “And this is going to be a tough period for the NCI, for cancer research, but it will come to an end.”
Sharpless’s remarks to BSA and NCAB follow:
Welcome to our first-ever virtual joint board meeting. This is an emergency meeting that I called to discuss the NCI’s response to the coronavirus pandemic. Thank you to all of you for making time. The pandemic has no doubt scrambled your schedules and I really appreciate your being available on short notice. NCI really needs your advice on some complex issues.
We’ll have talks by Doug Lowy, Dafna [Bar-Sagi] and Jim [Doroshow], and in a closed session Dinah [Singer] will have some further remarks. As noted, there will be time for discussion after the remarks, this is a vital part of today’s meeting. I’m sure we will all be saying many times today, “Could you please all mute?” as with my experience with prior WebExs.
One thing I want to make clear from the outset is that this is an emergency meeting to discuss the NCI response to the pandemic. And, necessarily, we’re going to be talking a lot about the coronavirus pandemic, but I want to make very clear right now that the primary focus of the National Cancer Institute is on cancer research and cancer care. That is our primary focus for now and forever. And this meeting will not supplant other scheduled NCAB or BSA meetings where we will continue to talk more about usual NCI business in those meetings.
I’d like to reiterate the points on the slide here that cancer research and cancer care remain job number one at NCI, even though our operations have been somewhat disrupted by the pandemic. And even during these difficult times, I think we are still making progress toward our mission of reducing cancer suffering.
“A moral obligation”
But today is an emergency meeting to talk about a crisis that has gripped our nation and disrupted our work. And I’m sure many of you would agree the National Cancer Institute has to be involved in the pandemic response. NCI has unique research capabilities and capacities, so, to help in this complex situation, we believe, is a moral obligation.


First off, the NCI has a long and storied history of intramural virology research, from Doug Lowy and John Schiller and Harold Varmus, to Bob Gallo to Sam Broder—pathbreaking, groundbreaking work on HPV and HIV and RNA tumor viruses—and to not use the virology expertise at the NCI during the current pandemic would seem to be a missed opportunity.
Also, the Frederick National Lab, which the NCI administers in collaboration with [the National Institute of Allergy and Infectious Diseases], has unique capabilities and resources that are really tailor-made for an emergency situation like this. The facilities at the Frederick Lab are quite exceptional, like the cryo-EM facility and the serology lab that can be useful and deployed in the current pandemic.
Frederick National Lab has unique contracting authorities that allow it to move very quickly to set up new research as needed. And it has the ability to form robust collaborative relationships, both with extramural scientists as well as industry. And so for these reasons it’s really well suited to take on the coronavirus pandemic. And Doug Lowy will be talking about many of the ways we’ve been using Frederick National Lab in conjunction with NIAID during the present crisis.
And then, lastly, the NCI supports the world’s best scientists bar none, and through our extramural funding programs, and that’s through our networks and our individual investigator-initiated grants, and these individuals have tremendous research capabilities and skills that can be very useful in a pandemic. So, not to involve the extramural fundees would seem, also, a missed opportunity. And we have heard a lot from you on this question.
I’ve had many conversations and emails with cancer center directors and scientists, with clinicians, with trainees at the various cancer centers about what you can do to work on the coronavirus pandemic and how the NCI can support those efforts. And thank you for giving us that feedback, and thank you for volunteering your expertise. In short, because of these reasons and others, we believe the NCI has important contributions to make during the coronavirus pandemic.
Operational updates
Just as the pandemic, no doubt, has changed operations at your institution, it has radically changed how the NIH and the NCI operate. We’re still able to keep research going while complying with physical distancing. One of our awesome WebExs is to do a senior weekly leadership meeting by this format and how well that works. We have suspended lab operations on campus and we have stopped all non-essential activities.
But the clinical center is still operational—treating patients, including cancer patients, with lifesaving therapies. It has reduced elective procedures and has taken in some COVID-19 patients, but it still continues to work, and NCI staff work there under, as you can imagine, difficult circumstances.
In order to reconfigure a 3,000-personnel organization with thousands of contractors in such a rapid capacity is really a challenge, but I’ve been thrilled and impressed by how much we’ve been able to do, even virtually. I’m also very excited to see how cross-government collaborations have sprung up in a very rapid and direct manner, both across the NIH and the rest of federal government.
In the last few weeks, the NCI has started very important mutual research efforts with NIAID, with [the National Institute of Biomedical Imaging and Bioengineering], with [the National Heart, Lung, and Blood Institute], and with the Aging Institute. We are also working very intimately with other federal agencies, including the FDA, the CDC, BARDA, and other parts of the HHS.
One other point I’ll make is that although the pandemic has disrupted operations, I believe we will take some very valuable and meaningful things from this experience. Some of the changes that are being inflicted upon us may actually lead to some good overall.
Two important examples: the first, I believe telehealth is here to stay. We’ve shown that, in a meaningful way, we can take care of patients via telehealth, and I predict cancer patients are going to like this in the future. They’re going to like the ability to see their doctor sometimes virtually, rather than in person.
And by the way, I will mention now that this is a tremendous pop-sci research opportunity. If you’re studying implementation science, your moment has arrived, because a thing like this where we’ve gone from nobody using telehealth to a large part of the country using telehealth—in, really, a couple of days—is a tremendous change in our practice, and really will lead to some great research, I believe.
Another area where I’ve seen a real example of something that, I think, will last after the pandemic, for the good, is the fact that the government can, when it needs to, move really quickly. We have been involved in complex multi-agency endeavors, but we’ve been able to really cut through a lot of the process and the usual steps to launch large, innovative, complex research efforts in a matter of days.
Jim Doroshow will talk about some of the clinical trials the NCI has recently stood up. I think these are some of the fastest trials that we’ve ever gotten started at the NCI in our history, and Doug Lowy will talk about many of the efforts at Frederick National Lab, including a serology effort they’re working with the FDA, it just has to be seen to be believed what they’ve started in just a few weeks (The Cancer Letter, April 10, 2020).
We also won’t cover everything the NCI is doing. It is just too much. We really have too many activities in this space, so I won’t really talk about our work with BARDA or what we’re doing in the SBIR program with small companies that work on coronavirus, or a very interesting set of collaborations with the NIBIB on a novel data platform that is aimed to help people get back to work.
But we will focus on a few of the more visible efforts in later talks. I hope that as life gets back to normal, we in the federal government can take these lessons we’re learning from the pandemic about how to do business differently and that will help cancer research in the future.
Resources for caregivers, patients
I’m pleased to report that the NCI’s Cancer Information Service, 1800-4-CANCER is fully operational and has been up continuously throughout the pandemic, even though it’s gone remote. We’ve already received hundreds of inquiries related to the coronavirus, as of yesterday. Most of the questions from cancer patients for their loved ones involve questions about risk and whether they are considered immunocompromised, whether their cancer puts them in increased risk.


As you can imagine, the nature of calls to 1800-4-CANCER really has changed during the pandemic. We get questions now like, “Should I go to my doctor? Can I get my scheduled chemotherapy? Can I get a blood transfusion?” I’m sure your institutions are dealing with these same questions. The Cancer Information Service is a highly visible service of the NCI that we provide for patients and it is moving along rapidly and working fully in a full capacity, even during the pandemic.
We’ve also produced some new key resources for patients and caregivers. A few examples are shown here. So, we stood up a coronavirus page with information for people with cancer as of March 13, that website has already received more than 60,000 visits. It’s the fourth most-visited page on our website. In addition, we have also stood up a coronavirus page targeted to researchers as of March 25, and that website has received 1,400 visits and we’ll provide these links in the material for the meeting and they can also be easily accessed from cancer.gov.
Extramural funding
In addition, we’re trying to maintain really strong communications to our research community. There’s been lots of internal communications. I did a virtual town hall meeting using the similar format to this that had 4,000 live attendees.
Here, I’m highlighting some of our external communications efforts: we’ve done cancer.gov websites, as I mentioned, we’ve had several blogs, we’ve done social media through many of our Twitter accounts, including the highly popular NCI Director account.


We really want people to understand what’s going on with grants and other funding matters. I had an NCI Bottom Line blog post on NCI funding during the coronavirus pandemic that’s received 5,500 visits since its publication on March 23, and it has some useful information for extramural fundees, and I commend it to all of you.
Also, Oliver Bogler has written a Bottom Line blog post about training grant issues, K awards, and F awards, and T awards and their deadlines and their reporting requirements, and how the NCI is going to handle those issues. That’s up now, and I commend it to all of you. In summary, we’re trying to maintain communications to all our stakeholders, NCI employees, researchers, caregivers, and most importantly, patients throughout the time of the pandemic.
The coronavirus has really affected how we do business at the NCI and, no doubt, how you do business at your institutions. But I want to reiterate right now, from an extramural funding point of view, we are fully operational. We are up and running, we can review grants, we can disburse funds, we can do what we normally need to do to support the extramural research community. But, no doubt, things have gotten more complicated, and we have received many, many questions from our investigators about grants, lab suspensions, and what this all means for them.
Cancer center directors, trainees, postdocs, integrated research programs, individual scientists have all been asking us lots of questions and I’ve listed some of the key issues here, like deadlines for applications and the use of funds and flexibility around reporting requirements and extensions for training periods. And let me say, I provided some material in advance from the Office of Extramural Research, Mike Lauer’s office at the NIH, that has a lot of really great information in that document, recently updated and is current, and I commend it to all of you, because it talks about a lot of these issues in detail.


Certainly, we can talk about any one of these more in a Q&A, if there’s interest. But I will say, as a general principle, the NCI is trying to provide maximal flexibility to investigators so they can get their important work done during this crisis. We really want to avoid work stoppages, we want to avoid layoffs, we want to avoid a loss of the research capacity for cancer research in the United States.
Although, it has to be acknowledged that the policies we adopt at the NCI have to fit within policies of the greater federal government, we cannot really go it alone on extramural grant policies, as what we do has to agree with what the NIH and other grant making organizations within the federal government do.
But when we do reach uniform agreement about these funding policies, the NCI is fully committed to disseminating that information as quickly as possible through blogs, our website, Twitter streams, etc.
It’s also important to note that we have a number of funding opportunities both not related to coronavirus, and I think those are out and probably familiar to many of you, and we also expect to have some coronavirus-related funding opportunities appearing soon, so please stay tuned for that.


We have some good news from a leadership point of view here at the NCI. Dan Gallahan, after being acting director of the Division of Cancer Biology for a while, has now become the director of the Division of Cancer Biology. We have really benefited from Dan’s leadership, and NCI is very lucky to have Dan in this role, which is tremendously important for the NCI. I would like to give a round of virtual applause for Dan Gallahan. Hey, alright, that worked!
I would also like to thank Dinah Singer, who held this position prior to Dan. She has now moved to become the deputy director of the NCI, and as I mentioned, we’ll be hearing from Dinah later on some important topics related to the NCI’s extramural programs.
On Capitol Hill
It is clear that Congress is extremely interested in our activities during the coronavirus pandemic. This is a hearing that was held on March 4—that was like a month ago—Labor-HHS subcommittee for the House Appropriations Committee, where there were a lot of questions about how the United States is responding. Doesn’t this really seem like a lifetime ago? I mean, here we all were, packed in a room, close together, not wearing masks, talking to each other. I had hair back then, that was a while ago.


Sitting beside me, by the way, is America’s most famous scientist, Tony Fauci [director of NIAID]. I think Tony and I have had a very close working relationship my entire time at the NCI, but it has really gotten a lot closer, because of the joint NIAID-NCI activities during the pandemic, and I think the nation as a whole is so lucky to have Tony’s leadership during this time. He is a remarkable American institution.
At this hearing, as you can imagine, there was a tremendous amount of questions about the coronavirus and the pandemic, but also this is the subcommittee, I remind you, chaired by Rosa DeLauro (D-CT) and Tom Cole (R-OK).
There was a lot of interest in cancer research. That group is very committed to cancer science and we had some great discussions about cancer research, paylines, pediatric cancer, clinical trials and many other topics. So, while Congress is very interested in coronavirus for the moment, they are consistently also very interested in supporting cancer research as they have done generously for a while.
I would say this congressional interest since this March 4 hearing has significantly even further intensified. Over the last week alone, I have spoken with, I think, maybe three or four senators and representatives about NCI activities related to the pandemic, and also with various staff for the House and the Senate, and these conversations really continue.


The Congress has done some stuff for coronavirus. Shown here are three fairly large supplemental spending packages that have moved rapidly through Congress to support a number of things regarding science and patient care, and the American economy. Most probably relevant for the NIH is phase 3, the CARES Act, which provided significant new money for the NIH as well as the FDA and CDC, and it also—an issue I’m sure very important to many of the board members—provided significant funding for hospitals, given the massive drop in revenues some hospitals are seeing with the cessation of elective surgeries and that type of issue.
Another thing we just learned recently is the FDA position regarding the CARES Act, which has a provision that all Americans can get testing for the coronavirus. And as I said, the FDA interprets that to mean both RT-PCR testing for the coronavirus as well as serologic IgG, IgM antibody testing for the coronavirus. This has very significant implications for the Frederick National Lab serology effort that Doug Lowy will be talking about later. There’s also talk, I’m sure many of you heard, about the possibility of a fourth supplemental spending bill. Should that happen, there is a good chance, I think, that there will be funding in that for the NIH and for the clinical center.
Progress in cancer research
I really couldn’t resist, as I said, even though you know it’s a lot of coronavirus going on around here right now, cancer really does continue at a brisk pace despite all the measures being taken to mitigate the pandemic, and I just wanted to highlight a few of those examples. These are things that have just happened in the last few weeks to give everyone a sense of how things are still moving along in the cancer research enterprise.
So, one about which I’m very excited is we enrolled our first patient on our CD33 CAR T trial. This is a trial for young adults and children with acute leukemia that has relapsed or refractory. And this is a first-in-man trial of a new CAR antigen and that reflects the work of Nirali Shah and collaborators at CHOP.
And that’s all important, but what is particularly remarkable at this trial in my mind is that the cells were made at our new Frederick National Lab facilities. So, that cellular therapies facility is open for business now.


We have a vision of doing several types of highly personalized cancer therapy for patients at Frederick National Lab, and I think the cellular program is just the beginning of that. So, I’d really like to congratulate Jim Doroshow and the Frederick National Lab team for getting this facility up and running so quickly.
The facility can make the CAR T cells there, and then ship them to a participating clinical trial site, in this case CHOP. And this technical advance is great news for kids and adults with leukemia, but I think we’ll see it spread to other CAR T trials soon.
This is a paper that came out from the intramural program from [Division of Cancer Epidemiology and Genetics] about a week or two ago, also with collaborators at NIA and CDC, and this shows a very strong association of steps per day with all-cause mortality.
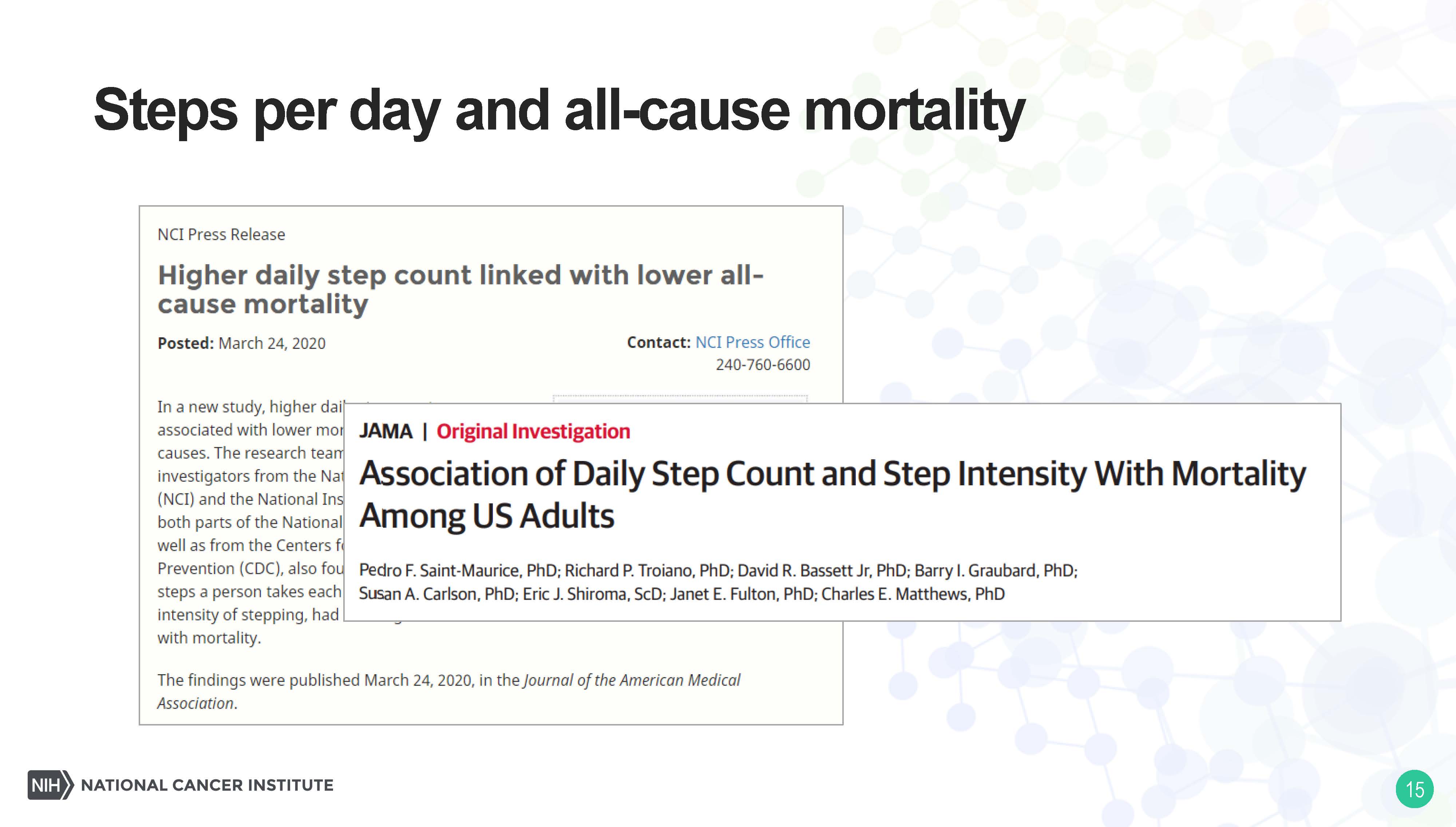

So, people who get 12,000 steps per day have a lower all-cause mortality than people who get 8,000 steps per day, who have a lower all-cause mortality than people who get 4,000 steps per day.
When I’m sheltering in place during a pandemic, this issue is really key. I’ve been trying to get out of the house to get my steps in, not just for my all-cause mortality, but for my mental health, and this great study was led by Chuck Matthews and others in DCEG.
This is a wonderful story 30 years in the making, 30 years of intramural research at the NIH about the use of selumetinib in NF1. It started with a fresh faced young geneticist named Francis Collins, who, while faculty at the University of Michigan, along with others, first discovered the gene NF1 that is mutated in this congenital pediatric cancer predisposition syndrome. And then people like Doug Lowy and others figured out what NF1 does from a biochemical standpoint and its role in Ras/MEK signaling.


And then a lot of studies, a number, over a decade of studies in the intramural program to try and address NF1 in patients. And those were largely led by Brigitte Widemann pictured here. And finally, after a lot of things that didn’t work, recently the NCI and Brigitte have developed this therapy that is really a notable success. It’s published recently in the New England Journal. This is not a cure for neurofibromatosis, but it’s incredibly meaningful for patients and vastly improves their quality of life. I really want to take my hat off to the people in the pediatric oncology grants who have developed this over so many years.
There’s just too much great science in the extramural community to mention it all and it’s so rapid and staggering in its output. I thought I would show one slide that I particularly liked, which is a story from my old friend Sean Morrison’s lab showing this interesting relationship between metastasis and melanoma spread.
Metastasis is one of the great unsolved riddles of cancer research, and I think science like this that helps us understand the cellular basis of that process is really, really key, and is a good example of why basic research is what really moves the needle, in my opinion, for cancer patients over the long term.
And this is why I’ve been such a fierce defender of the RPG pool my entire time, because it produces great basic science like this, and I believe someday we’re going to be able to prevent metastasis because of studies in this vein.


“Battalions of sorrows”
So, let me close now. I really won’t sugarcoat our present circumstances. This epidemic is bad, and it’s going to continue to be bad for a while, especially the next few weeks. This period of waiting for some normalcy to return has made me think a lot about what it was like when I was a leukemia doctor.
In leukemia, in acute leukemia, you give patients a big bolus of chemotherapy, and then you wait four to six weeks for them to recover their bone marrow and go home. And induction chemotherapy, as many of you know, involves a lot of waiting and a lot of anxiety, hoping for a return to a more normal time.
And this period now reminds me a lot of waiting for bone marrow to return and the inpatient service while we’re waiting for this pandemic to abate. And in particular, I’ve been thinking about a former patient from that time. He was an English professor who taught undergrads English literature, and he’d gotten his induction chemotherapy, and was waiting in that hospital for his bone marrow to recover, so he could go home.
Now, a little-known fact is that I was an English major for about a month, as an undergraduate, before I realized how much writing an English major entails, and then I switched to become a math major. But I’ve always loved literature, and I’ve always taken the chance to learn from my patients. So, when I would come in every morning with my huge team of residents, medical students and pharmacists to round on this patient, we would always ask him for some great thought from English literature to summarize his day.
This guy had an amazing memory, and he never disappointed in producing these sonnets and couplets on the spur of the moment, always with something that fit the mood of the day. And it kind of became a fifth vital sign. We’d have his blood pressure and his heart rate, and his thought for the day from classical literature, and we could tell when he was doing better or worse based on what he said that day.
And one morning, on a bad day at the nadir of his chemotherapy, right after he’d received several pieces of bad news, he gave us a little known quote from Hamlet: “When sorrows come, they come not single spies, but in battalions.”
And I’ve been thinking about that a lot lately. I see these stories about ICUs full of patients in New York, and I imagine what it’s like to work in that situation, and I just can think of nothing but battalions of sorrows.
But I’m here to tell you we’ll get through this, just like my team and I got that guy through his induction chemotherapy—he went home in remission, back to a more normal life. And this is going to be a tough period for the NCI, for cancer research, but it will come to an end.
And I want to thank everyone again for their time and for what each of you are doing at your own institutions to address this pandemic, in the tragedy of the current set of circumstances, but also to continue to make progress against cancer, an ancient and terrible disease that causes immense human suffering in its own right.