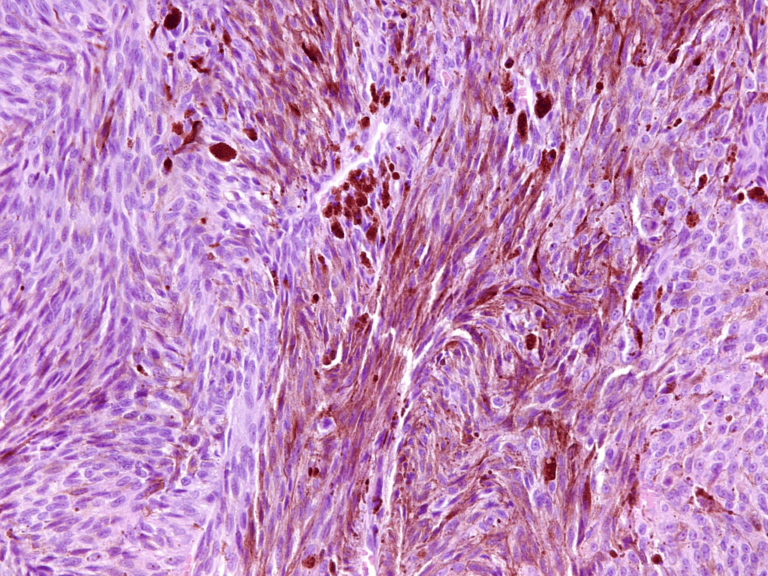
On a single day in March, Dr. Bernard Fisher of Pittsburgh, the country’s pre-eminent breast cancer researcher, saw his own career crumble, and watched helplessly as the research organization he had led through unprecedented advances in the treatment of breast cancer was abruptly shut down.
It was a shattering experience for the scientists who had spent decades on the work. And for women around the country who suffer from this deadly disease, it was a disturbing setback.
These dramatic developments were the result of another doctor’s misguided actions, years ago and miles away. A Montreal surgeon — one of about 5,000 doctors to join Fisher’s study group — had begun to falsify the paperwork of some of the patients he enrolled in several studies. Mostly, they were small changes in the dates that determined whether women met the deadline for enrolling in the studies. His actions, which involved 99 women out of the nearly 34,000 in North America who participated, did not seem to change any of the important medical conclusions the studies reported.
Fisher’s staff discovered the deception in 1991 and reported it to federal cancer officials, who had funded the experiments for several years. Then, this spring, the story burst into public view when it was printed on Page 1 of a Chicago newspaper. Not long after the headlines, Fisher was fired and the study was put in limbo.
The Montreal doctor’s actions were clearly scientific misconduct. But some wonder if the punishment exacted on the research effort was too harsh for the crime.
Was the severity of the penalty simply an effort to maintain the credibility of a medical experiment? Or was it the inevitable result of a struggle by three powerful institutions — science, politics and journalism — to decide who should police medical research?
What really happened here? Was it fair? Did it help anyone? This four-part series tells the story behind the headlines…
Discovering fraud in breast cancer research: A gradual process
The young assistant stared at the papers she had just pulled from the file.
“Look! There are two of them!” said Teresa Wright, in bewilderment.
Dr. Ann Brown, a clinical biostatistician at the National Surgical Adjuvant Breast and Bowel Project in Pittsburgh, leaned over to take a look at the papers, which had come from St. Luc’s Hospital in Montreal.
Something did seem odd, she thought.
Instead of just one photocopy of a medical report on a breast cancer patient enrolled in one of the NSABP’s studies, there were two of them, exactly alike, except for one critical fact:
One record said the patient had undergone breast cancer surgery on June 19, 1987, while the other said the date was June 29, 1987.
Depending on which date was right, the patient would either have been eligible to enroll in the study, or ineligible.
Errors were sometimes found in the hundreds of thousands of pieces of paper that flooded through the NSABP’s offices every year. But on this summer day in 1990, instead of a smudged date, or a dictated patient report that didn’t match the original hospital chart, here were two copies of the same document, with different dates neatly typed on each one.
What was this? Brown thought, a dart of worry piercing her.
When she showed the documents to her supervisors, they were equally mystified.
But Walter Cronin, the NSABP’s deputy director, wasn’t hearing alarm bells yet.
“I figured, gee, maybe there was something different about the way the folks at St. Luc’s kept records,” he would say later. “They were French-speaking, after all.”
Disaster in the making
It wasn’t a language gap.
The discovery of the unmatched twin records would lead, four years later, to a scandal that would strike fear in thousands of women with breast cancer.
It would lead to the abrupt dismissal and public humiliation of one of the world’s pioneers in breast cancer research, Pittsburgh’s Dr. Bernard Fisher.
And it would severely cripple one of the world’s most prominent, innovative, and productive breast cancer research organizations, an organization Fisher had helped found.
But no one at NSABP had any reason to imagine any of those agonies in June 1990 when first confronted with the discrepancy of one number on a piece of paper from St. Luc’s.
St. Luc’s Dr. Roger Poisson, one of Montreal’s leading breast cancer surgeons, was a major contributor of patients to NSABP’s studies, and had been praised repeatedly by Fisher for his efforts.
So, while the Pittsburgh staff was puzzled, they were not alarmed. Surely, they thought, this could be explained.
But their concern deepened in September 1990, when Cronin conducted an audit of records at St. Luc’s and found more data discrepancies, plus irregularities in women’s consent forms. Clearly, something wasn’t right, but Fisher — the head of the study — still wasn’t told.
It wasn’t until November, according to Fisher, that Carol Redmond, his chief biostatistician and closest aide, walked into his office and told him there were “irregularities” in Montreal.
Fisher said that Redmond, who declined to be interviewed for this story, was adamant that “one had to be sure before one made any accusations against anybody. To make any accusations without being sure, you were opening yourself up to a suit,” he said.
So, on Dec. 7, Fisher and Redmond met with Poisson and his wife, Sandra Legault-Poisson, in Pittsburgh.
In a memo she wrote later, Redmond said that she and Fisher told the Poissons that there were problems with their data and with information on patients’ consent to join experimental therapy trials.
They told them a more intensive site visit would be undertaken “as soon as schedules permitted, after which, we would evaluate whether any additional problems that might be uncovered indicated the need for further actions.”
Poisson would say later that the meeting “chagrined and saddened” him but he didn’t tell Fisher at that point what he had done.
On Dec. 21, NSABP’s Cronin sent a memorandum to Redmond, reporting two cases in which St. Luc’s had provided followup information on patients who had already died.
Cronin added, though, that “in our judgment, there is no evidence of intentional falsification of data.”
That opinion would soon change.
Vrai and faux
When Cronin and two other auditors returned to St. Luc’s in January 1991, they found alterations in five more cases out of 120 they reviewed.
On the third day of their visit, Cronin picked up two reports on a breast cancer patient. Like the ones Wright had found in Pittsburgh, they were identical except for one item — there were two different readings on a lab test.
And then he saw something else.
The first report had a yellow label stuck on it that said “vrai.” The other report was labeled “faux.”
Cronin’s heart sank. Poisson had kept two sets of files, labeled with the French words for “true” and “false.”
Cronin turned to the other two auditors, Marge McLaughlin and Larry Wickerham. “Look at this,” he said quietly.
Without a word to Poisson, the three NSABP auditors left St. Luc’s and somberly boarded a plane to Pittsburgh to tell Redmond the bad news.
Fisher said he wasn’t notified that his staff had found clear evidence of falsification until February 1991. He was devastated.
“I had no frame of reference relative to this situation, fraud or anything like that,” Fisher said. “All of my research life, I’ve practiced and preached credibility and honesty.”
When he went home that evening, Fisher had a strong sense of foreboding. He remembers telling his wife that “some time, it would come back to haunt us.”
On Feb. 8, 1991, Poisson sent a letter to Fisher acknowledging the falsifications. Fisher immediately got on the phone and notified National Cancer Institute officials, who funded most of NSABP’s research.
A week later, Fisher sent NCI a detailed letter about the St. Luc’s falsifications, and eight days after that, he met personally with NCI staff. He also notified the Office of Scientific Integrity (OSI), which investigated scientific misconduct allegations, as well as the U.S. Food and Drug Administration and the Office for Protection from Research Risks, a separate agency that works to ensure that study participants are not endangered.
All these actions met NCI guidelines, Fisher stressed, and afterward, “Dr. Redmond and myself, we felt very good about what we had done.”
What took so long?
The subsequent investigation revealed that Poisson had been fudging his records since 1977.
Why did it take 13 years for the NSABP to discover discrepancies in Poisson’s records?
In the early years, Poisson only falsified a handful of cases—a date change here, a date change there. The majority of falsifications would come later, and once the problem became “pervasive,” NSABP officials said, they caught it during routine auditing procedures.
The other reason Poisson may have escaped detection for so long was that he didn’t tamper with records once a woman had been enrolled in a study.
When Poisson altered a woman’s file, it was usually to change the date when a woman’s biopsy or cancer surgery had occurred to help her get into a study past the official deadline.
Fisher has been exasperated by charges that NSABP should have caught Poisson much earlier.


Being able to detect a small number of eligibility-date changes in the early years would have been “like looking for a needle in a haystack,” Fisher said.
Looking back on the problem, however, NCI officials now say that his argument is faulty. NSABP’s auditing was insufficient, they said, because it still took several years to catch the falsifications after most of them had occurred, and that was in part because NSABP wasn’t looking at enough files.
“It was always eight charts (that were audited), whether the center was big or small,” said Dr. Bruce Chabner, director of the Division for Cancer Treatment at NCI.
The eight-chart rule met NCI’s guidelines at the time, but the agency was trying to get NSABP to audit more files at each center.
That would have increased the odds that the problem would have been detected more quickly, federal officials said.
But when it was their turn to investigate Poisson, federal investigators moved at a glacial pace.
During the nearly two years it took for them to look into the case, everyone was forbidden to discuss it.
“I don’t know why it took so long,” said Dr. Jules Hallum, who was OSI director at the time. “We were constantly understaffed and we had other investigations going on, too.”
Also, he said, “there was a period of time when we had no travel money.”
At one point, OSI investigator Dorothy McFarlane left the NSABP case to work on another project for several months. To add to the confusion, the OSI moved its offices and some staffers were laid off and then rehired.
Phone calls went back and forth sporadically between McFarlane and the NSABP’s Redmond in an effort to reconcile the facts, Fisher remembered, but he never sensed any urgency on the part of federal investigators.
Finally, in December 1992, the newly renamed Office of Research Integrity finished its investigation.
Out of 1,054 cases examined at St. Luc’s, the investigators found 115 fabrications or falsifications affecting 99 patients, all but one related to eligibility.
When to tell the public
At that point, the existence of fraud at St. Luc’s had been well established for two years, but no one outside the NSABP, the NCI or the Montreal hospital knew about it.
The scandal would stay quiet for another year — in part because Fisher had not yet published a reanalysis of his studies, excluding the bad data.
Fisher and his critics disagree on why it took him so long to do the reanalysis.
In January 1993, two Cancer Institute officials wrote to NSABP and said that the federal report on the fraud would be released in a few weeks, and Fisher’s group should be prepared to publish a scientific report on the matter shortly afterward.
The ORI findings were released a month later, but there was no report from Fisher.
Fisher said, however, that he did have a plan to get the word out, one that was developed by Redmond.
First, he would present a technical analysis of the fraudulent data at a May 1994 meeting of the NSABP members in Nashville, and follow it with a commentary on its significance. Then, there would be a written report published in a scientific journal.
It would be a careful, deliberate approach—the way Fisher had always done things.
Fisher said he felt no pressure from NCI. In fact, he said, NCI didn’t contact him again in writing about publishing his reanalysis until October 1993.
NCI officials tell a different story.
In an interview in The Cancer Letter, a newsletter published in Washington D.C., Samuel Broder, the NCI director, said the agency had received “very strong assurances from Dr. Fisher that he would be writing a reanalysis, and as it turns out, that wasn’t the case.
“Don’t tell us you’re going to publish a paper,” Broder said, “and then have us patiently asking you, ‘Can you please let us know … ?’ If you say you’re going to reanalyze, reanalyze promptly. Do it. Don’t give us thousands of reasons why not.”
Still, even though Fisher hadn’t published his reanalysis, the news did start to seep out—but not exactly on the front page of The New York Times.
The first reference to the fraud investigation came in ORI’s own newsletter in the early spring of 1993. Another report appeared in the June 21 U.S. Federal Register, the official federal publication of agency regulations and findings.
A New York science newsletter, Probe, also carried a short story on the matter in September 1993. Its editor, David Zimmerman, had tried to reach Fisher in August, but each time he called, Fisher directed his staff to tell Zimmerman he was out of town or unavailable. Eventually Zimmerman gave up.
Fisher felt no need to go public with the information.
After all, there had been no health crisis. Fisher’s staff had already determined that taking out all of Poisson’s patients would not change the fundamental outcome of the NSABP studies.
He also didn’t feel compelled to call any of the scientific journals in which previous studies had been published, including what was now known to be fraudulent data.
“When you get no change in the results,” Fisher said, “you don’t call up the New England Journal of Medicine and say, ‘Guess what? Nothing happened!’”
Enter Suzanne Hadley
As 1993 came to a close, Poisson’s fraud had managed to stay underground for nearly three full years.
That would soon change.
Shortly before Christmas, Suzanne Hadley bumped into a lawyer from the Office of Research Integrity.
Hadley was well known in Washington D.C. as a determined crusader against scientific misconduct. She had spearheaded many of the major investigations into science fraud in recent years, first as deputy director of the Office of Scientific Integrity, ORI’s predecessor, and then, working with Michigan Rep. John Dingell, who had made scientific misconduct one of his priorities.
Hadley had been involved in the investigation of Poisson’s fraud when it surfaced.
Then she had started working for Dingell, and became deeply involved in the investigation of NCI’s Dr. Robert Gallo, who had been accused of falsely claiming credit for discovery of the AIDS virus. The primary journalist working on that story was the Chicago Tribune’s John Crewdson.
On this December day in 1993, her former colleague, the ORI attorney, told her his office had a case “where the investigation was concluded a long time ago and it was clear there was fraud and it was clear that a number of (published scientific) papers contained the fraudulent data,” she recalled.
He went on to say that “we can’t get the investigator to publish corrections and tell the world about it.”
When she asked which case it was, she was told, “Roger Poisson.”
Hadley was dumbfounded.
She couldn’t believe that the Poisson case was still unresolved.
She told her colleagues on Dingell’s Oversight and Investigations Subcommittee, and, in early January 1994, they met with ORI officials.
Hadley discovered at that meeting that nearly a year had passed since ORI had first asked the National Cancer Institute to ask Fisher to publish his reanalysis.
“It was pretty clear that little or nothing had been done” since that time, said Hadley, who is no longer working with the subcommittee. “Should ORI have followed up with NCI? Should NCI have followed up and done something? No question. There’s plenty of blame to go around.”
Another month-and-a-half went by.
Then, on March 13, the Tribune’s Crewdson wrote a front-page story on Poisson’s fraud—the first major media attention it had received.
Hadley said she didn’t know how Crewdson learned about the Poisson fraud, and Crewdson declined to talk about the matter.
Once the news hit, Hadley wasn’t surprised at NCI’s reaction.
“This thing didn’t happen in a vacuum,” she said. “NCI had been on a slow burn with Bernard Fisher for close to two years,” she said, because it wanted speedier audits and independent reviews of data quality.
“I think in some ways NCI was just waiting for something.”
When the headlines hit, federal officials flew into action.
Fisher’s years of achievements crumble overnight
Atlantic City, 35 years ago.
On the same stage in the same auditorium where Miss Americas paraded, preened and wept, a contest of another sort was taking place.
It was a medical conference, the American College of Surgeons’ annual meeting. All the great names in breast cancer surgery were on the dais, including Jerome Urban, legendary surgeon from Memorial Sloan-Kettering Hospital in New York City, and Cushman Haagenson of Columbia University, author of a classic text on breast diseases.
Both were staunch defenders of the radical mastectomy—the removal of the entire breast and adjacent pectoral muscles whenever a tumor was malignant.
Before them stood a younger researcher from the University of Pittsburgh named Bernard Fisher, tall, with a rubbery grin like Walter Matthau’s, uttering the unspeakable words:
The radical mastectomy, Fisher said to his colleagues on the stage, was unnecessary. Less disfiguring surgery would do the job just as well.
When Fisher finished and came off the stage and began to make his way through the crowd, suddenly, a young medical resident, a disciple of Haagenson’s, lunged out of nowhere and grabbed him by the lapels.
“How could you say those things to my teacher . . . !” he hissed at Fisher before the two were separated, while the crowd oohed in horror and delight.
“I thought he was going to punch me,” Fisher said, remembering the incident with a certain glee.
Hounding the heretic
Beating up on Bernard Fisher—at least verbally—was a popular sport for members of the American surgical establishment in the 1950s and ’60s.
Surgeons were raised to think of Bernard Fisher as the bogeyman.
Craig Henderson
Even though he eventually would be acclaimed for his accomplishments in breast cancer research, in the early days of his career, Fisher was a renegade.
A “dissident surgeon,” thundered Haagenson in his writings, warning Fisher’s supporters that they risked “ruination of the soul” if they followed him.
“Surgeons were raised to think of Bernard Fisher as the bogeyman,” said Craig Henderson, a noted breast cancer oncologist at the University of California at San Francisco, “and these things take a long time to die.”
Fisher’s sin was to question the radical mastectomy, a procedure introduced in the late 19th Century by William Stewart Halsted. Surgeons knew it was mutilating, but they felt it was necessary if one were to “get it all.”


But Fisher believed that cancer cells spread systemically through the body’s blood and lymph vessels, instead of by inching through surrounding tissues—a theory that would be incorporated into standard medical practice by the mid 1980s. Because of that, Fisher reasoned, less disfiguring surgery, with radiation, would be just as effective as removing the whole breast.
By 1994, the “Fisher Hypothesis” had revolutionized breast cancer treatment, bringing him worldwide acclaim.
In some ways, he was like Pittsburgh’s other medical superstar, liver transplant pioneer Thomas Starzl.
Like Starzl, Fisher has won almost all the major prizes in scientific research. And like Starzl, Fisher is a charismatic, larger-than-life personality, a loner with many admirers but few close friends.
The similarities end there, however.
Starzl, who needed to scare up money and military jets for expensive transplant operations, often courted the media.
But Fisher ducked the limelight. He liked to let “the science” speak for him, and didn’t particularly trust reporters to translate scientific information correctly.
Had it not been for the fraudulent data controversy that rocked his career in his 76th year, it’s entirely possible Bernard Fisher would have lived out his life in peaceful anonymity, lauded in medical circles, but hardly a household name.
The thrill of adventure
As a boy growing up in Squirrel Hill, Fisher showed a natural scientific bent, perhaps influenced by a great uncle who was a physiologist and surgeon at Case Western University at the turn of the century. He also credits Lon Colburn, a chemistry teacher at Taylor Allderdice High School, with inspiring him.
Then, too, there were the tough expectations of his father, Reuben “Ruby” Fisher, a traditional, no-nonsense son of a Jewish immigrant from Lithuania who ran a successful produce business.
The elder Fisher banned his two sons from the premises of the business, determined that Bernard and Edwin would be the first in his family to go to college.
“You damn well went to school and you damn well performed,” recalled Edwin Fisher, a noted Shadyside Hospital pathologist who’s a tougher-talking version of his older brother.
In the early 1900s, Ruby Fisher, “King of Potatoes,” was successful enough to move out of the North Side to what was then suburbia—Squirrel Hill, where the Fisher boys were born.
For the Fisher brothers, it meant stickball on the streets, the Pittsburgh Pirates at Forbes Field, and a bird’s-eye view of the Ringling Brothers Circus tent from the third-floor window of their house.
Occasionally confined to his bed during outbreaks of scarlet fever or whooping cough, Bernard Fisher pored through books about adventurers like Richard Halliburton—“spitting off the Matterhorn, the longest spit in the world!”—or Admiral Byrd’s trek to the North Pole, or best of all, “The Microbe Hunters,” a classic book about early microbiologists and their discoveries.
In 1936, Fisher entered the University of Pittsburgh, and three years later, its medical school, graduating in 1943.
An ulcer precluded him from serving in the war, so he began his career as an intern at Mercy Hospital.
By the time he had married Shirley Kruman, a bacteriologist at West Penn Hospital, he knew what he wanted to do with his life.
Research.
Learning about cancer
It was a logical choice for a man who had spent his youth devouring books about adventurers, because scientific research seemed to be another way to conquer the unknown.
For the next 20 years, in the 1950s and 1960s, Fisher spent most of his days in a laboratory, often joined by his brother Edwin.
The 1950s were his “Promethean period,” he liked to say. Just as the ancients were riveted by the myth of Prometheus, whose liver was devoured by an eagle at night but grew back during the day, Fisher wondered: How could it be that a damaged liver could grow back to normal size and then stop?
Eventually, that would lead him down another path—into the biology of tumor growth. After all, it was the other side of the coin. A liver stops growing at a certain point, but a tumor never stops.
One day in 1957, Fisher’s work was interrupted by a telephone call from his mentor, I.S. Ravdin, chairman of the department of surgery at Penn, who asked his former student to drop everything and come to Washington, D.C., for a meeting.
Fisher went reluctantly, hating the distraction.
It was at that meeting at the National Institutes of Health that Ravdin announced his intention to form something called the National Surgical Adjuvant Breast Project.
Unwieldy as the title was, it meant what it said.
Ravdin and his colleagues at the NIH wanted to launch a federally funded program to evaluate the effectiveness of “adjuvant” therapy, or anti-cancer drugs, after surgery for early breast cancers, unlike the prevailing practice of using the drugs only on seriously ill patients.
The proposal interested Fisher only slightly.
“I said, ‘Oh, what the hell, OK,’” he would go home and do the study.
Well-behaved disease?
Once he joined NSABP, Fisher’s reluctance evaporated in light of a startling discovery: next to nothing was known about how cancer cells grew and spread.
Until that time, it had been assumed that the cancer spread in an orderly fashion, that it was “a well-behaved disease that spread centrifugally, or locally, before it metastasized anywhere else in the body,” said Fisher’s colleague, Dr. Janet Wolter, a Chicago breast cancer surgeon.
But results in the operating room didn’t seem to confirm the local-spread theory.
No matter how much of the tumor and surrounding tissue doctors removed, survival rates remained the same, Wolter said. So “Fisher finally said, cancer is not a well-behaved disease.” After much experimentation, he concluded that it spread through the blood and lymph vessels, and if it did, it might be just as effective to do conservative, limited breast surgery combined with radiation to stop the disease.
The only way to test this thesis was through clinical trials, where one group of women would get a mastectomy, and the others would get more conservative surgery.
Fisher soon became a “clinical trials zealot,” as he put it.
When he was made chairman of the National Surgical Adjuvant Breast Project in 1967, the first thing he did was move the project’s headquarters to his home town of Pittsburgh.
Then, he began setting up trials that would test his theories.
It was tough going at first, because many of the most prestigious research institutions wanted nothing to do with Fisher’s experiments.
So Fisher became a traveling salesman, making his pitch at smaller clinics and community doctors’ meetings around the nation, from Johnstown and Oil City to Saginaw, Mich., and Wichita Falls, Texas.
Gradually, the gravelly voiced Pittsburgher with a knack for persuasion made converts, enrolling enough patients to begin the first comparative surgery study in July 1971.
One group of patients would receive standard treatment, which at the time was the radical mastectomy. The other group would receive a “simple” mastectomy, where only the breast was removed but not the pectoral muscles, a slightly less mutilating procedure.
Acclaim, then the end
That first study was successful, and Fisher still considers it his personal landmark, even more than the later lumpectomy trial.
But it didn’t win him quick respect.
In 1974, when Fisher reported the early results at a National Cancer Institute conference, showing the effectiveness of the simple mastectomy, “we were flushed with success—for about 12 hours.”
The next day, the press ignored his claims and his colleagues trashed him.
“He was treated abominably,” recalled Samuel Hellman, a prominent radiation oncologist at the University of Chicago, and one of those who still opposes Fisher’s theory that cancer spreads systemically.
Slowly but surely, though, the NSABP and Fisher began to gain broader credibility.
As one successful study followed another, more and more doctors joined the NSABP, and Fisher and his staff began attracting awards, fellowships, grants and invitations to speak.
Yet even by 1985, more than 15 years after he took over at NSABP, Fisher still wasn’t accepted by some in the establishment.
He and his supporters still fume at what they say was the New England Journal of Medicine‘s one-year delay in publishing his landmark lumpectomy study that year.
“It was held up by people in the surgical establishment who were opposed to the idea of a lumpectomy,” said Canadian surgeon Richard Margolese. “But they couldn’t find anything wrong with the manuscript, so they finally had to publish it.”
But New England Journal Editor-in-Chief Jerome Kassirer disputes that account. “I’ve heard that story many times before and it’s nonsense. It’s just not true. We asked them to get more followup data and it took them that time to get it.”
By the early 1990s, the NSABP included about 500 institutions and about 5,000 doctors.
Its expansion dovetailed with the growing strength of the women’s rights movement.
At first, Fisher’s work was lauded by breast cancer activists for pushing the American medical establishment toward lumpectomies.
But the relationship started deteriorating in 1992 when Fisher began what he called his legacy—a huge 16,000-woman study that would test whether the drug tamoxifen could prevent the onset of breast cancer.
Some activists openly challenged him, worried about giving a drug with toxic side effects to health women. They disliked his reaction.
“The moment he found out we had criticisms of his trial, he would never talk to us again,” said Cynthia Pearson, director of the National Women’s Health Network in Washington D.C., recalling a hearing on the prevention trial held by the Food and Drug Administration.
After one woman in the audience stood up and asked that Fisher’s tamoxifen study be delayed until scientists had 10-year results on the safety of the drug, Pearson said, Fisher snapped at her.
“He got just livid and ended up shouting at this woman, ‘How long do you want to wait?’” Pearson said.
At around the same time, some of Fisher’s colleagues began to wonder when he would turn over the reins at NSABP.
In 1991, a “pink sheet” published by a National Cancer Institute peer review group auditing the NSABP praised Fisher, but asked if he shouldn’t start thinking about the “next generation” of leaders.
Fisher, 73 at the time, told the panel that his plan was to leave once his breast cancer prevention trial got under way sometime in the mid-1990s.
“I guess the problem with me is that despite my age, my enthusiasm never ran down, and I’ve never been told by others that I’m mentally incompetent,” he said later.
“But I’m no imbecile. I knew I wasn’t going to live forever or be here forever.”
Still, he felt he was at the top of his game.
But the rules of the game had changed. There was more and more government oversight, more pressure not to make mistakes. Fisher also watched with distaste as other medical institutions got research grants by catering to the media, something he would not do.
In an oddly prescient speech before the American Society of Clinical Oncologists in 1993, Fisher warned that “politics, personalities, process, publicity, media coverage, fiscal concerns and other secondary considerations must not be permitted to take on a life of their own, and like a cancer, destroy our true mission.”
It was a warning that would soon turn into devastating reality for Fisher and the NSABP.
Fisher describes ordeal as “reign of terror”
As spring approached this year, Dr. Bernard Fisher was at the height of a brilliant career. At the age of 75, he had spent more than half a century building his reputation and accumulating nearly every major medical award for his work with breast cancer.
Revered for his achievements and his integrity, he held an unchallenged spot in the medical pantheon.
Until March 13.
On that day, a story in the Chicago Tribune revealed that a Montreal surgeon at St. Luc’s Hospital had supplied fraudulent data for more than a decade to breast cancer studies done by Fisher’s National Surgical Adjuvant Breast and Bowel Project.
The speed and the vehemence of the negative reaction to the story stunned Fisher. He was in a fog, trying to adjust, trying to focus.
A planned 70th birthday party for his wife Shirley was canceled. His daughter Beth, a Charlottesville, Va., doctor, was home for a visit. Faced with the chaos, she decided to stay on and help her father.
For the next two weeks, Fisher would undergo what he called “a reign of terror” by officials from the National Cancer Institute, people with whom he had been friendly for years.
It started on March 18, at 5:30 on a Friday afternoon, when Fisher got a frantic call from Richard Ungerleider, chief of the clinical investigations branch at the NCI.
Your paperwork shows there are problems with patient records at Louisiana State University and Tulane University, Ungerleider told him. Send your top people down there to do audits by Monday morning and suspend the universities from the study, he told Fisher.
Fisher dispatched his most knowledgeable staffers.
Two days later, Fisher, accompanied by his daughter, met with officials at the University of Pittsburgh, where Fisher’s research project was based. The NSABP was an independent organization, but its research money was funneled through Pitt.
Pitt officials had just learned about the Montreal fraud through the Chicago Tribune article because Fisher, who had known about it for three years, had not told them.
Dr. Thomas Detre, Pitt’s senior vice chancellor for health sciences, didn’t seem overly concerned, Fisher recalled. “It was just a discussion of what could this be about? How could this thing take place?”
A decision was made to do nothing publicly and to wait and see what happened next.
The next day, Monday, March 21, “all hell broke loose,” Fisher said.
The fax machine started spewing paper and never let up, he said. The requests came primarily from NCI and the office of Michigan Congressman John Dingell, who was planning to hold hearings on the fraud.
“They’d give you 10 demands—all information about this and that—and we want this by close of business, and all the staff was running like crazy, and it was like something out of Charlie Chaplin,” Fisher said.
NCI was feeling the heat, too.
Staff members of Dingell’s committee, known for their investigations of scientific misconduct, “were all over us,” remembered Dr. Bruce Chabner, director of the Division of Cancer Treatment at NCI. After the Tribune story broke, he said, “there were a series of interviews in which every aspect of this trial was called into question, both the supervision by NCI and the execution by NSABP.”
As chief of the division overseeing the NSABP grant, Chabner said he was ”very distressed and embarrassed” about the whole episode.
Peoples’ jobs were on the line, and not just Fisher’s.
“The stakes were very high, scientifically and personally,” added another NCI official. “Everybody was concerned for their own scientific careers, for greater or for more narrow reasons.”
A humiliating visit
More faxes to Fisher followed, and then came a phone call, alerting Fisher that he would be visited by Chabner and Ungerleider.
When the NCI contingent showed up in Pittsburgh, Fisher felt helpless. The two people who could answer most of NCI’s questions, Larry Wickerham and Walter Cronin, were in Louisiana auditing LSU and Tulane, at NCI’s insistence.
The NCI “wanted files on this, wanted files on that,” and Fisher, without his two top aides, couldn’t accommodate them. A recent move from another part of the building had complicated matters.
As a result of the disastrous visit, NSABP was put on probation.
And the demands continued to pour in.
“We were working 18 hours a day, and nothing was going on. We were trying to fulfill these orders, and it was just chaos,” Fisher said.
Pitt’s specially hired lawyer on the matter, Martin Michaelson, tried to soothe Fisher, suggesting at one point that he read poetry. Michaelson also emphasized his strategy—keep quiet, don’t say anything, and it will all blow over.
But it didn’t. It was a big story—in fact, it would be listed as one of the top 10 stories of the year, according to the Associated Press.
To Fisher, though, the media coverage seemed unfairly negative. One Pittsburgh television newscaster solemnly reported that Fisher himself had been accused of falsifying data—something that was never true.
They “were making these accusations that were blatantly false, that we were just derelict in this and derelict in that. I wanted to get up and shriek and say, ‘No we weren’t!’
“But the university policy was, ‘Keep quiet, it’ll go away.’ “
Why the strategy of silence?
The primary goal, Fisher said, “was not to provoke John Dingell.”
By now, the powerful Michigan congressman’s presence loomed like an ominous thundercloud.
Dingell was known for his rough treatment of witnesses who came before his subcommittee. No one was immune: Nobel Prize-winning scientists, CEOs of major corporations, Navy admirals. A small cottage industry had sprung up in Washington—lawyers specializing in counseling witnesses ordered to appear before Dingell’s committee. They even had an informal name: the Dingell bar.
‘I’ve never heard of him’
All of this was new to Fisher.
“I’d never heard of John Dingell, didn’t know anything about him,” Fisher said. But after he was told about what happened at Dingell hearings, Fisher began to feel real fear.
The fateful moment for Fisher came on March 25.
Looking through the NSABP files, an NCI official found a Sept. 22, 1993, report on a visit to another Montreal hospital, St. Mary’s.
The report said the NSABP auditing team had found a major problem with one chart, in which a mammogram date for one woman apparently had been changed. The finding, according to the auditors, “presents a serious problem.”
But the audit report had never been forwarded to NCI. It remained in a file cabinet in Pittsburgh.
Chabner said later that this single file was what prompted NCI’s insistence that Fisher be replaced as principal investigator for NSABP. After the fraud committed at St. Luc’s by Dr. Roger Poisson, after reports of missing files in Louisiana, after learning that no audits had been done by NSABP for months, it was just too much.
“There was a sense that the NSABP was clearly in danger of collapse,” said Dr. Michael Friedman, the director of NCI’s cancer therapy evaluation program.
“It was clear that Dr. Fisher was being overwhelmed by the workload.”
And yet, with the exception of the St. Mary’s file, NCI officials had been aware for years of all the problems they later cited when they fired Fisher.
But in the frantic climate following the Tribune story, amid all the telephone calls from Dingell’s office, those previous problems looked much more serious to NCI.
It was Friedman who made the decisive call to Fisher on Monday, March 28. The two already knew each other well.
They had worked closely when Fisher was president of the American Society for Clinical Oncologists the year before.
Fisher took the call in his office. Also present were his daughter Beth; Al Ciocca, a Pitt lawyer; and NSABP’s chief biostatistician, Carol Redmond.
Friedman was on his speaker phone, joined by Chabner and several other NCI officials. NCI Director Samuel Broder was also in the room at NCI headquarters in Bethesda, Md., but he did not speak.
Fisher remembered that Friedman sounded agitated.
We’ve found out you knew about the St. Mary’s audit, and didn’t do anything, Friedman told Fisher angrily.
Fisher said his staff had never told him about the St. Mary’s audit until it was discovered by the NCI official. That didn’t placate Friedman.
This will tear down research all across the country, Friedman said, over Fisher’s protests that he didn’t know what Friedman was talking about.
Fisher still remembers the words that ended his distinguished 35-year tenure at the NSABP.
“You’re finished, Bernie!” Friedman yelled. “You got (screwed) by your staff. You’re out!”
Pitt jumps in
On March 29, NCI, in a letter, officially ordered Pitt to remove Fisher as principal investigator and appoint an interim replacement, citing “a litany of NSABP failures.”
Besides the fraudulent data, NCI cited NSABP’s decision to halt audits at member hospitals, delays in establishing independent boards to monitor patient records, and Fisher’s slowness in publishing a reanalysis of his studies excluding the tainted information.
The NSABP office was formally placed on probation until corrections were made. As part of that, it was ordered to immediately adopt a “rigorous” schedule of audits of patient data, and to suspend enrollment of new patients in various studies.
Fisher was given no opportunity to defend himself in a hearing, and Pitt officials were presented with only two choices: Comply with NCI requirements, or give up NCI grants to NSABP, which totaled about $22 million per year, about $10 million of which went to Pitt.
They’d give you 10 demands—all information about this and that—and we want this by close of business, and all the staff was running like crazy, and it was like something out of Charlie Chaplin.
Bernard Fisher
Pittsburgh Cancer Institute Director Dr. Ronald Herberman—a laboratory scientist who specialized in immunology and knew little of breast cancer clinical trials—was appointed by Pitt to head the NSABP.
It was a shotgun marriage, and it was shaky from the start.
The NSABP might be headquartered in Pittsburgh, but it was actually an international network of about 5,000 surgeons and researchers. They had always prided themselves on their accomplishments and independence. Now, they believed, Pitt’s Herberman was co-opting their studies and treating them like errant children.
On the evening of March 30, a grim NSABP executive committee met in Pittsburgh.
Fisher, their leader and inspiration for more than 20 years, spoke first. He simply told his colleagues that he was no longer chairman. Then he left.
Herberman took over the meeting. One of the committee’s first acts was to vote unanimously for Fisher’s reinstatement—hardly a warm welcome for the new acting chairman.
It would be one of many volleys fired between NSABP committee members and Pitt in the succeeding months, culminating in an acrimonious lawsuit.
“It was not inevitable to lose, irrevocably and forever, the goodwill of leaders of the NSABP, who very naturally had a loyalty to and respect and admiration for Dr. Bernard Fisher,” said Dr. Yosef Pilch, a longtime NSABP member.
But Pitt did lose that goodwill, he said, because its officials “overreacted in a very paranoid fashion to pressure from NCI,” particularly on auditing patient records.
The employees at NSABP headquarters felt the same way. After years of working with Fisher, whose style, if occasionally overbearing, was also inclusive and open, they found themselves abruptly put under the yoke of Pitt’s new management, which was a more top-down, hierarchical structure.
A problem with numbers
NSABP’s new management was immediately under the gun, as Dingell’s staff pushed it and the NCI to get ready for the congressman’s first scheduled hearing on the fraud, less than two weeks away.
And even though Fisher had been ousted, he was still being ordered to produce documents for NCI or the Dingell committee.
The queries were neither tactful nor sympathetic.
On March 30, the day after his firing, a shell-shocked Fisher went to his office at Pitt’s Scaife Hall, where he received a fax from NCI demanding to know the number of St. Luc’s patients in each paper that NSABP had published or was planning to publish.
“Please fax this information by tomorrow afternoon,” it said.
Fisher had just sent one list of papers with the St. Luc’s data the day before. By the end of March 30, he had added seven more to the list.
One of the stickiest problems arose over a paper Fisher had submitted to the NCI’s own Journal of the National Cancer Institute. That paper, scheduled for publication in April, had included the St. Luc’s data, but Fisher hadn’t mentioned that fact until NCI officials ordered him to detail it in a footnote.
The dispute over that paper symbolized a larger problem that continues to this day.
What is the proper way to deal with the St. Luc’s data in published studies? Poisson was found guilty of altering records on 99 patients out of 1,511 he had enrolled in various NSABP studies.
In scientific papers including St. Luc’s patients, should only the falsified cases be excluded, or should all of them go? Should all NSABP papers be published with two sets of statistical tables, one with and one without the St. Luc data?
NCI officials wanted to throw out all the St. Luc’s patient data, but NSABP staff in Pittsburgh resisted, citing support from prominent statisticians.
They saw no reason to discard patients whose records were in order. Such a move would void the contributions of hundreds of Montreal-area women who had volunteered to participate in the studies, they said.
Another bone of contention was the “rigorous” audit schedule demanded by NCI.
It was more complex than it sounded, requiring not just “standard” audits, involving a sampling of files—but “for cause” audits that required scrutiny of each patient’s record, in Louisiana, New York and other sites where there seemed to be problems.
The NCI wanted every NSABP study with a potential for fraud to be re-examined.
But its first priority was the landmark 1985 lumpectomy study, which showed that conservative breast surgery, combined with radiation, was just as effective in treating early breast cancers as the more disfiguring radical mastectomy.
NCI wanted an intensive audit of the major institutions involved in the study to be done before the April 13 Dingell hearing.
To meet that deadline, the NCI sent teams of eight to ten people to each of 40 institutions in the U.S. and Canada. The teams had been culled from the ranks of pharmacists, Ph.D.’s, oncologists, nurses and others who did not necessarily have experience with either clinical trials or breast cancer research.
A Passover debacle
For some, the audits bordered on the absurd.
Dr. Richard Margolese, principal investigator at Jewish General Hospital in Montreal, said an NCI auditing team showed up unannounced at his hospital on the first Monday of Passover, asking to see records dating back to the 1970s.
The auditors were pleasant, even apologetic, Margolese said. “But, I must tell you, the auditing process was a shambles.”
Charts and records of patients—some of whom had moved or had died—had to be retrieved from community doctors’ offices, brought to Jewish General, and stacked on the floor. At one point, Margolese said, a stack fell over and records got mixed together.
The auditors stayed all week, then told Margolese his records were in good order.
“The word used was ‘pristine.’ “
Five days later, though, the auditors were back to look at what they described as “missing data,” Margolese said. They wanted to review all 135 charts from the lumpectomy study.
The second visit lasted one day, and Margolese—who had been out of town—met the auditors as they were preparing to leave. “They said they had six ineligible charts,” Margolese recalled, but then assured him they considered that a low number.
“I told them, ‘I don’t think six is a low number.’ “ Margolese insisted they go over the charts together. He was able to immediately show that all but one of the women was eligible.
Still, for reasons he doesn’t know, Jewish General was barred a few weeks later from enrolling patients who had signed consent forms before April.
Margolese was never formally notified, and only learned of the suspension when the center tried to enroll a patient two months later and was told it couldn’t.
Finally, after NSABP intervened, the enrollment ban was lifted.
While the auditors were scattering around the countryside, the man who started it all held a news conference in Montreal.
Roger Poisson was not apologetic.
He derided “those people in their ivory towers” who had criticized him for fudging dates on eligibility criteria. “It’s all very well to compare clinical experiments carried out in the laboratory,” he said. “I was on the battlefront with patients who were dying.”
Poisson’s defense—that his falsifications were minor and in the best interests of the patients—was almost universally rejected.
But he was rapidly becoming irrelevant, a quaint sideshow to the real issue at hand: the upcoming Dingell hearing.
On April 5, Donna Shalala, the Secretary of Health and Human Services, weighed in with a point-by-point 12-page response to a list of questions from Dingell’s staff.
Shalala offered her assurance that the NSABP study conclusions would hold up, but added that “neither my office, the NCI, nor (federal science fraud investigators) is satisfied with the handling of this matter.”
She promised changes.
She was deferential to the congressman. Most Washington bureaucrats were,because of Dingell’s power to make or break them. During the testimony to come, not one of them would stand up for the man who is, arguably, the world’s greatest breast cancer researcher.
His “nonobservance” turned into a major fraud case
Roger Poisson can still remember the first time he fudged a a breast cancer patient’s medical record, on a day long ago in 1977, so she could be enrolled in a study even though she had missed the deadline by several days.
It was just a small deceit, really. A quick change of dates, so that the woman could meet the study’s requirement to be enrolled within 30 days of her diagnosis. It was all “in the best interests of the patient,” as the Montreal researcher described it in a recent interview.
That little deception, of course, was followed by another. And another. Until all the little deceptions had snowballed into one giant case of scientific fraud, causing the near destruction of the National Surgical Adjuvant Breast and Bowel Project, the world’s largest breast cancer research organization.
But even today, Roger Poisson still doesn’t quite understand what the fuss was all about.
After all, what he did wasn’t really fraud, Poisson said, just “a nonobservance of strict criteria that had no oncological value.”
Three years after his falsifications caused his removal from the NSABP, and nine months after the scandal became public, Roger Poisson, 63, appears to be a man at peace with himself and with his actions.
Despite losing his access to U.S. grant money, to his professorships at the University of Montreal and his position as chief of oncology at St. Luc’s Hospital, Poisson still has a thriving breast cancer surgery practice—“thousands of patients,” he says, a touch of defiance in his soft, reedy, French-accented voice.
In my mind, I was thinking that the good I was doing was by far more important than the small irregularities.
Roger Poisson
Even after he was blackballed from American-funded research for eight years, Poisson was not fired from St. Luc’s, because, officials said, they found no proof that he had harmed patients.
And despite the worldwide disapproval that rained down upon him last spring in the wake of the scandal, Poisson says—and other Montreal colleagues confirm—that he has become a hero to many in the French-Canadian community because of a belief that he was scapegoated by U.S. bureaucrats.
The stories about his falsifications seemed suspiciously timed, he thought, appearing simultaneously everywhere from South America to Eastern Europe last March.
“How do you explain something so well-orchestrated?” Poisson said. “It’s clear that some people wanted my skin.”
Another explanation is that news services are able to move a story around the globe within minutes.
Whatever the world thinks of Roger Poisson, he believes he did the right thing by breaking the rules.
“In my mind, I was thinking that the good I was doing was by far more important than the small irregularities” he committed.
In all, investigators from the U.S. Office of Research Integrity found that Poisson had been responsible for 115 separate instances of data falsification involving 99 patients in 14 breast cancer studies from 1977 to 1990.
Most were minor, such as changing the date of an operation to make a woman eligible for the study; a few, however, were more serious, including one in which the nature of a breast tumor was deliberately misrepresented as less advanced than it actually was. Another involved a woman with cancer in both breasts who had been classified as having cancer in one breast.
Poisson had a ready explanation for each infraction:
- Of the requirement Poisson most frequently flouted, that a patient be enrolled within 30 days of diagnosis, Poisson said it was an artificial, arbitrary deadline that was later changed to 56 days during the course of the study.
- Of the NSABP staffers’ discovery of documents labeled true and false in his files, “one data coordinator did that for about four or five patients,” Poisson said, a trace of impatience in his voice. “Why? I can’t say. As the principal investigator, do you think I was supposed to supervise everything? They blew that out of proportion.”
- Of the incident in which he described one woman’s breast cancer as less advanced than it actually was in order to get her into the study, he said the patient actually had “a slight edema,” or swelling, in one breast, but years of experience told him that she would still benefit from being in the study.
- Of the patient classified as having cancer in one breast, resulting in her having radiation of that breast, while she was actually afflicted with cancer in both breasts, Poisson pointed out that she also had chemotherapy, which treated both breasts’ tumors.
“Roger Poisson would not have changed serious things, like (enrolling) a patient without a cancer, or (enrolling) fictional patients,” Poisson said of himself. “None of that has been found in my files.”
He said changing dates to make some women eligible was like “crossing against a red light at 2 o’clock in the morning.”
Others disagreed.
The federal Office of Research Integrity barred him from performing any U.S.-funded research for eight years, the stiffest penalty ever imposed in a scientific misconduct case, and the U.S. Food and Drug Administration barred Poisson for life from access to experimental drugs.
Later, he said the worst pain was losing the confidence of NSABP Chairman Bernard Fisher, a man he considered almost a father figure.
“It came to me like a death,” he said, of Fisher’s dismissal of him. “I had no warning.”
For his part, Fisher remembered Poisson as “a pleasant enough guy, who was devoted to what was going on, a disciple of what it was we were trying to do.”
Fisher never thought there was anything suspicious about Poisson’s behavior. Under NSABP’s funding system, Poisson enrolled so many patients that he wasn’t paid on a per-case basis, but received a flat amount of grant moneyfrom the National Cancer Institute—so money wasn’t an incentive, Fisher believed.
Unbeknownst to Fisher, though, Poisson was extremely frustrated whenever he couldn’t enroll a woman in a study because of what he considered a technicality.
It often takes a long time to convince a woman to enter an experimental trial, Poisson said.
“You talk to her, she goes home, talks to her husband, she calls you and says, ‘I don’t know,’ and then finally, three weeks later, she agrees to participate.
“And then you look at her medical history and realize that she is two days past the deadline—within 30 days of diagnosis—for enrolling.
“So what am I supposed to do? Tell the woman, I’m sorry, forget it, after all the pep talks? I’m sorry, I did not have the courage to say that to a woman.”
Poisson actually thinks his fraud may have helped, in the end, because it led to publicity about the value of lumpectomies.
Fisher’s outlook about Poisson’s role is less positive.
“The guy did what he did, and as far as I’m concerned, that’s his problem,” he said. “The hell with him.”
Fisher feared Dingell inquiry
On Wednesday, April 13, Rep. John Dingell, one of the most powerful congressmen on Capitol Hill at the time, began another of his dramatic scientific misconduct hearings.
In the past, the Michigan Democrat had put such famous scientists as AIDS researcher Robert Gallo and Nobel laureate David Baltimore in the heat of his spotlight.
This day, the target would be Pittsburgh’s Bernard Fisher and his breast cancer research group, the National Surgical Adjuvant Breast and Bowel Project.
But Fisher would not be present for the first hearing.
The day before, there had been an announcement that Fisher was ill, and had decided not to testify.
But Fisher wasn’t sick.
That was a cover story devised by a University of Pittsburgh lawyer, who thought it was not the right time yet for Fisher to go public.
The strange turn of events had begun when Fisher met for four hours the week before in Washington with Dingell’s staff to go over his testimony.
At the meeting, Fisher “seemed shellshocked,” one Dingell staffer remembered.
“Everybody was trying to help him put the pieces together, of what he had done, what he hadn’t done. We were trying to help,” the staffer said.
Fisher went back to Pittsburgh and spent the weekend in seclusion, preparing his testimony.
“He wanted to tell his story. It was written from his soul,” his daughter Beth recalled.
But when a draft of Fisher’s testimony was faxed to Pitt’s lawyer, Martin Michaelson, the day before the hearing, word came back to Fisher that Michaelson didn’t like anything about it. Michaelson didn’t think it had come close to accepting enough blame for what had happened.
Thus began a debate between Fisher and the Pitt lawyers. Should he testify, or should he not? Maybe it was best to keep quiet.
Michaelson decided that Fisher should not attend, and that he would cite ill health.
Joseph Onek, whom Fisher had hired as his personal lawyer, remembered concurring with the decision.
“We just didn’t know enough” about the allegations against the NSABP, he said. “It didn’t seem like a good time to do this.”
A charismatic witness
Even without Fisher, the hearing received national media coverage.
Two hours after it was over, Dingell’s staff crowded around a television to watch the network coverage of the hearing.
What they saw was the earnest face of Jill Lea Sigal, a 32-year-old Virginia woman who told the world of her own breast cancer diagnosis six months before.
An environmental consultant, Sigal had worked extensively on Capitol Hill for the previous 11 years. So when she first saw the news that a Canadian surgeon had falsified data in some of NSABP’s studies, she knew what to do. Sigal immediately called a congressman whom she knew who put her in touch with Dingell’s staff.
Sigal told a Dingell staffer that she was furious with Fisher and the agency that funded the studies, the National Cancer Institute, for its lax oversight.
The staffer said, “Well, if we have a victim’s panel, maybe we’ll want to use you.”
Later, another staff member called, asked her more questions and then said, ”You’d be the perfect witness.”
And she was.
Sigal’s angry words rang through the hushed committee room and on televisions across America.
Although she hadn’t participated in the lumpectomy study, she had relied on its findings, she told the House Oversight and Investigations Subcommittee. After consulting with her physicians, she decided to have only the lump and a small amount of surrounding tissue removed from her breast.
Now, she was outraged—outraged at the falsification of records, and outraged that the information about it was not available when she was making life-or-death decisions about her own treatment.
I don’t mean to say there weren’t any problems that shouldn’t be corrected. But a lot was made out of it, and it had the effect of not only frightening women, but making it harder for women to participate if they have this image in their mind about fraud.
Diane Walsted
“How many women must now wonder, as I do every day, if they will diebecause they may have made the wrong decision?” Sigal asked.
Afterward, Sigal was approached by Bruce Chabner, a top NCI official, who complained that she had needlessly frightened women into thinking they had opted for the wrong surgery. Furious, Sigal told Dingell about Chabner’s remarks, prompting NCI Director Samuel Broder to send her a letter of apology.
Yet for all Sigal’s righteous indignation over Chabner, he was simply relying on the best information scientists had—that the basic findings of Fisher’s original lumpectomy study were correct.
Two days after the hearing, in fact, Edward Sondik, acting deputy director of NCI, sent out a “Dear Colleague” letter describing a reanalysis that had been done by a government-hired contractor of the lumpectomy study and two other NSABP breast cancer studies.
His conclusion: Discarding the falsified data from the one Montreal hospital “has no substantive effect on the main study findings.”
The message was confusing. Television images of angry breast cancer patients were juxtaposed against repeated scientific assurances that the studies were valid.
A sense of proportion
Indeed, for every Jill Sigal, there was a Diane Walsted.
“It seems like it got blown out of proportion,” said Walsted, a 52-year-old breast cancer survivor who volunteers on a hotline for breast cancer patients in Chicago.
“I don’t mean to say there weren’t any problems that shouldn’t be corrected. But a lot was made out of it, and it had the effect of not only frightening women, but making it harder for women to participate if they have this image in their mind about fraud.”
Another scare for some women was the news that a few patients who took the anti-cancer drug tamoxifen as part of an NSABP study had died after contracting uterine cancer, and that Fisher had delayed putting that information on patient consent forms.
Dingell and some patients were angry at the delay. But that feeling wasn’t universal.
Dr. Peter Eisenberg, of Marin Oncology Associates in Greenbrae, Calif., said women at his center weren’t shocked by the new information about uterine cancer deaths.
The existing consent forms already listed uterine cancer as a possible side effect of tamoxifen, he said. To say some of those women eventually died was not surprising.
“In fact,” he said of his patients, “they couldn’t understand what the hubbub was all about.”
To Sharon Green of Y-ME, a national breast cancer support organization based in Chicago, one could look at the controversy in terms of “A-problems, B-problems and C-problems.
“A-problems are just messiness,” she said. “A-problems are not going to affect outcomes and are not going to hurt anyone’s life. B-problems are a little more serious. And C-problems are the serious ethical and scientific problems.”
Her assessment of the NSABP controversy: “My guess is, we have more of the A- and B-problems.”
Certainly, the falsified data, the poor record-keeping, the unclear documentation on getting informed consent, the delays in telling the public—all these concerned Green.
But she wondered: “In reality, did it really matter?”
Troubles for Pitt
When Fisher had been summarily fired from his post as chairman of NSABP in late March, Pitt officials had stepped in to take over the vast research organization, which involved about 5,000 doctors and 34,000 patients.
By late April, Pitt was having its own problems with the federal government.
NCI officials were pushing for a quick “recompetition” of the NSABP grant so that other medical centers could make proposals to take over its cancer research.
That would cost Pitt more than $20 million a year in federal funding, and would take away control over the massive, 16,000-woman breast cancer prevention trial that NSABP had begun.
Then Pitt got a little breathing room when the NCI’s Board of Scientific Counselors balked at the idea and urged that Pitt be given time to fix the NSABP’s problems.
In the meantime, NCI had thrown Pitt another curve.
The agency wanted the university to investigate Fisher and Carol Redmond, his chief biostatistician and closest aide, on whether they had been guilty of improper behavior by knowingly submitting research papers containing some of the falsified Canadian data.
Up to that moment, Fisher and Redmond had not been accused of doing anything that was scientifically unethical themselves. Now, they, too, were being tarred with the damning phrase “scientific misconduct.”
One of the papers involved a tamoxifen study and included some women whose records had been altered by Montreal surgeon Roger Poisson.
Fisher made an intriguing argument on why it was proper to leave those cases in the study. Two of the Montreal women later contracted uterine cancer and died. If he had excluded the cases where data had been falsified, Fisher said, he would also be throwing out important information on the side effects of the drug.
A top federal cancer official took a different view.
“To include systematically fraudulent cases … there’s no other field of research where you would do that,” said Dr. Bruce Chabner, director of the Division of Cancer Treatment at NCI.
Chabner said it was important for Fisher to acknowledge the falsified data, so he directed Fisher to contact several medical and research journals, including the New England Journal of Medicine, which had published NSABP’s landmark 1985 lumpectomy study.
But the New England Journal balked at publishing Fisher’s reanalysis of the lumpectomy study, saying it wanted to wait until NCI was finished auditing the NSABP records.
NCI had asked Fisher for a year to publish the reanalysis. Now that he was finally ready, he couldn’t get it into print.
Eventually, the federal Office of Research Integrity took over the investigation of whether Fisher and Redmond had engaged in misconduct. Today, eight months later, no decision has been made.
On the outs
By now, Pitt’s relationship with Fisher had grown muddled and tense.
One of the lawyers who would help Pitt investigate Fisher was Martin Michaelson, the same man whom Fisher had taken into his confidence after the scandal broke, who had perused Fisher’s files and who had suggested that he read Kipling and Tennyson to calm his spirits.
Fisher was stunned that a lawyer who knew so much about him would now be investigating him.
Pitt’s treatment of Fisher didn’t sit well with some at the university.
“A lot of people look at this and say, ‘If you can go after people of the quality of Bernie Fisher, you can go after anyone,’” said Dr. Lewis Kuller, a longtime colleague and head of the Graduate School of Public Health’s Department of Epidemiology.
Still, Pitt said it was trying to find a way to retain some role for Fisher in NSABP’s studies without further angering federal officials.
University officials had initially proposed that Fisher be kept away from any administrative duties, but be allowed to serve as scientific director of the project.
That would recognize his brilliant contributions as a researcher and appease the hundeds of doctors in the United States and Canada who regarded Fisher as the heart and soul of NSABP.
But Dingell’s staff, which was getting ready for a second hearing on the breast cancer fraud, was adamant that Fisher no longer be part of NSABP’s administrative hierarchy.
That message was relayed to Pitt officials by NCI, and the university announced that the new NSABP would have no formal role for Fisher.
Pitt made one last show of public support for Fisher and Redmond.
It came after U.S. Sen. Arlen Specter appeared at a news conference at Pitt on May 16.
The Philadelphia Republican promised to push to get NSABP’s suspended studies restarted.
Afterward, Jeffrey Romoff, president of Pitt’s medical center, said the university had asked NCI to consider allowing Fisher and Redmond to have a role in the project.
His comments were printed the following day at the top of a front-page Post-Gazette story headlined, “Pitt Fights Back.”
Nine days later, NCI officials sent a letter to Dr. Ronald Herberman, a Pitt official serving as interim chairman of NSABP, asking whether Pitt’s statements were true.
“Because we have not yet received the formal request referred to in Dr. Romoff’s statement, please inform us as soon as possible of the University of Pittsburgh’s position on this matter,” it read.
Chabner said he later received a call from Pitt in reply.
“Someone said ‘I’m sorry. We didn’t mean to say that. It was a mistake,’ “ he said.
‘Not enough groveling’
If any question remained that Pitt was backing away from Fisher, it seemed settled when Pitt officials asked to testify separately from Fisher at the second Dingell hearing on June 15.
By then, many of the initial scientific controversies that had erupted in March had diminished.
Nevertheless, the hearing did deliver high drama—the long-awaited face-to-face meeting between Dingell and Fisher.
For Fisher, it was a total, unmitigated disaster, the low point of his life.
One detail in particular sticks in his mind.
The night before the hearing, he was in his hotel room at the Willard in Washington, D.C., with his wife Shirley,and eldest daughter, Beth, a University of Virginia doctor who had taken a leave of absence to assist her father.
The telephone rang.
It was Joseph Onek, the Washington lawyer whom Fisher had retained.
As was the custom, Fisher’s testimony had been forwarded to the Dingell committee, and the committee staffers had indicated that there was a problem, Onek said.
“They said there isn’t enough groveling,” Onek told him.
While Onek later confirmed that account, a Dingell staffer who declined to be identified strongly disagreed with Onek’s interpretation.
The real problem with Fisher’s testimony, the staffer said, was that “they really couldn’t come to grips with admitting the warts and wrinkles of the project.”
In either case, it was clear that Dingell’s staff wanted some acknowledgment of mistakes from Fisher.
They certainly got that admission from Pitt officials.
Dr. Thomas Detre, the university’s senior vice chancellor for health sciences, preceded Fisher at the hearing and talked about how major universities historically had treated senior researchers like Fisher gingerly, a “culture of deference” that he believed should change.
Fisher was up next.
For the following two hours, he endured withering questioning from Dingell and other subcommittee members.
Reading from his prepared statement, Fisher emphasized that “there was never any intent to hide information regarding the discovery of falsified data at St. Luc Hospital.”
He apologized for not having published a reanalysis of the studies yet.
“We did not realize that the failure to publish our findings immediately would be misinterpreted by the public as an indication that we were concealing information,” Fisher said.
Of the controversy over the uterine cancer deaths, he said, “it might have been possible to collect and report information about these deaths sooner, but there was never any intent to withhold information.”
Then, in a statement that he added after the “not enough groveling” remark by Onek, Fisher conceded that “perhaps my passionate attention to the science overshadowed my administrative insight, and this was a mistake. I should have been firmer with the personnel responsible for the audit program” that checked patient data.
Although he said NCI officials “have been involved in every aspect of our efforts,” Fisher did not read a subsequent sentence from his prepared statement:
“Consequently, NCI must share with the NSABP responsibility for deficiencies in our project.”
Mary Otto, a writer for Knight-Ridder newspapers, later described Fisher as “tired, abstracted and ill-prepared” during the hearing.
Widespread problem?
Much of Dingell’s unrelenting inquisition centered on whether patient data problems existed at other hospitals, beyond St. Luc’s, where Poisson had worked.
The congressman said they did.
At one site, he said, “three-quarters of the patients enrolled did not meet the eligibility criteria.”
Fisher answered that there “may be some misunderstandings regarding clarification of ineligibility.”
Later, as Fisher was explaining the NSABP audit process, Dingell cut him off, and repeated: “One site had three-quarters of the participants ineligible.”
“I am certainly unaware of that, sir,” Fisher replied, his voice cracking. “I really am not aware of it.”
Dingell then listed the centers with “problems with either fraud or slovenly work”—South Nassau Communities Hospital in Oceanside on New York’s Long Island, Rush Presbyterian Hospital in Chicago, St. Joseph Hospital in Lancaster, Pa., and Pitt.
At the University of California-Davis, Dingell said for the third time, three-quarters of the patients were ineligible.
It was a dramatic drilling. But it wasn’t true.
Dr. James Goodnight, director of the UC-Davis Cancer Center, said later that a sample audit of eight charts had found possible problems with six of the patients’ records.
But there was never evidence that three-quarters of all 184 patients at UC-Davis had errors in their records.
A closer look at the other centers cited by Dingell also reveals less than meets the eye.
Pitt’s Herberman said he was unclear what problems Dingell was talking about at Pitt, other than some records that had come in late.
At South Nassau, two of 207 patients had been found to be ineligible. The error had been caught by an NSABP audit in 1992 and the women were removed from any studies. Since then, South Nassau had enrolled only one more patient.
A spokeswoman at Rush Presbyterian said there were irregularities on a single audit in 1991, but she could give no further details.
Joan Hess, of St. Joseph Hospital in Lancaster, said its inclusion in the list “was all in error.”
“We checked this out and what we ended up getting was a written apologyfrom … the University of Pittsburgh,” she said. “Our files were up to date. We had no idea how we were named.”
Dingell also cited “serious and chronic problems” with data at Tulane and Louisiana State universities at the June hearing.
Eventually, though, those problems turned out to be much less serious.
The first reports intimated that large numbers of ineligible patients might be at both sites.
Dr. Roy Weiner of Tulane said there were “very real problems,” but they weren’t ethical—they were administrative. Over the 17 years that the Tulane-LSU group had been in NSABP, Weiner said, the office staff remained at two people, even as the number of patients in studies soared to 450.
The staff simply couldn’t keep up the records on all those women, and so auditors had to search files in doctors’ offices and clinics to find the information verifying that women were eligible.
While not all patient data was found, Weiner said, “some of the deficiencies were truly trivial, and in many instances, the data that was missing was never even required” for the study. Since then, he said, Tulane has beefed up its staff to eight people.
Dingell smiles on Pitt
Between his first and second hearings, Dingell underwent a noticeable change in attitude toward Pitt.
At the first hearing, Dingell had hinted he might want to look into other scientific misconduct cases that had occurred at the university in the past.
By the second hearing, though, Dingell was solicitous toward Pitt officials who testified, including Chancellor J. Dennis O’Connor, Detre and Herberman. Dingell praised Pitt as “a great institution, one of which you are justifiably proud.”
In the weeks leading up to the hearing, Dingell’s staff had wanted a pledge that Pitt would live up to its “institutional responsibility” to take care of problems at NSABP, Herberman said.
He said O’Connor, Pitt’s top administrator, wrote to NCI Director Samuel Broder, “providing very strong and unequivocal assurances” that Pitt recognized the problems and was committed to fixing them.
Fisher was becoming more and more isolated.
After his fumbling performance at the second Dingell hearing, Fisher went home with his family, numb with grief.
“We were sitting shiva,” his daughter Beth said, evoking the Jewish tradition of mourning, as she described the black mood in the Fisher household as friends dropped by to try to lend support.
Still dazed from Dingell’s harsh treatment, Bernard Fisher faced the prospect of building a defense against Pitt’s investigation of him.
He figured it was time to get new lawyers. He hired John Bingler, a member of Thorp, Reed & Armstrong, and James Lieber, a member of the law firm Lieber & Hammer in Shadyside.
Bingler and Lieber wrote to Pitt, complaining about how Pitt’s special lawyer, Michaelson, had unfairly started out as Fisher’s attorney and then became involved in the investigation of Fisher over misconduct allegations.
They got no response.
So, on a humid day in early July, Fisher called a news conference in his lawyers’ office and announced he was suing the university, a place he had called home for most of his adult life.
“Now is the time when this whole thing has got to stop,” Fisher said.
He wanted his job back and he wanted the university to halt its investigation.
One month later, he was joined in the federal lawsuit by members of his executive committee. They thought their action would force a quick responsefrom Pitt.
Instead, it led to protracted, unfruitful settlement negotiations between lawyers for Fisher and Pitt officials.
At one point, a settlement agreement was drafted by Fisher’s attorneys that would have made Fisher scientific director for NSABP. It remained unsigned.
The ongoing talks became an albatross for the NSABP.
The project had selected Dr. Norman Wolmark, a respected breast cancer surgeon from Allegheny General Hospital, to become the new leader of NSABP.
As NCI director, Broder had to approve Wolmark’s appointment before he could begin. But Broder wouldn’t do that as long as the suit was pending.
Eventually, committee members realized they had to get back “on line” with NCI or face possible extinction.
Nothing showed the change in attitude more clearly than a meeting of the executive committee in Bethesda, Md., headquarters city of NCI, in November.
Present were Fisher and his brother Edwin, a longtime research associate. Some committee members then asked: Did it serve NSABP’s interest to continue in the Fisher lawsuit?
The question was rhetorical, but its implications, coming from a group of Fisher’s most loyal supporters, were far-reaching: NSABP was ready to move forward, with or without Bernard Fisher.
Fisher affair clouds future study
As the new year draws closer, Bernard Fisher waits.
He waits for the completion of a federal investigation into studies he published. He waits for the resolution of his lawsuit against the University of Pittsburgh. He waits, most of all, for vindication.
At 76 years old, with his spirits flagging and his legal bills mounting, he feels precious time slipping away.
The pre-eminent breast cancer researcher is cut off from the important work that has consumed his life.
Each day, he still goes to work at his old offices in the University of Pittsburgh’s Scaife Hall. But instead of analyzing data that might lead to medical advances, Fisher confers with lawyers, writes defenses of his actions and takes calls from colleagues expressing sympathy.
The breast cancer studies he once directed six days a week for a quarter of a century are being run elsewhere on the campus. It’s a short walk away—but it might as well be another galaxy.
This is what Fisher has come to in the nine months since the world learned that a Canadian doctor had falsified data used in several of Fisher’s studies.
His eldest daughter, Beth, is always by his side. A Virginia doctor, she took a leave of absence to help restore her father’s reputation. During his interviews with reporters, she takes notes furiously, quick to jump in with corrections if her father stumbles or a reporter makes the wrong assumption.
Recently, Fisher ran into an old friend.
“The guy said to me, ‘What do you do? What are you doing now? You go to work every day, but you don’t have access to this, or that? What are you doing?’” Fisher said, mimicking the man’s nagging voice.
“Well,” Fisher said quietly, “that’s a good question.”
With no meaningful scientific work to do, he is a king without a court.
Epilogue: Other scientists
The humiliation that Fisher has undergone, and the failure of Pitt and the National Cancer Institute to stand by him, have sent shock waves through the scientific community.
If it could happen to him, many believe, it might happen to any scientist who is ambitious enough to tackle large and complex research projects, but might be a little too arrogant, or stubborn, or slow to respond to demands by federal agencies.
As a result of Fisher’s ordeal, scientists once again are debating who should police science and how to do it fairly.
The federal Office of Research Integrity, a little-known department working out of the Department of Health and Human
Services, is responsible for investigating reports of serious misconduct.
But because the office is understaffed and underfunded, investigations often drag on for more than a year. Scientists are forbidden from discussing the case publicly until a conclusion is reached.
Despite the gag order, the biggest cases often are played out in front of a national audience long before the formal probe is completed. That occurs when the staff of the House oversight and investigations subcommittee decides it, too, will investigate.
No other nation in the world has been so committed to clinical trials, and the American taxpayers have a right to ask that we monitor and successfully administer such trials.
Mace Rothenberg
In the past, the subcommittee’s involvement often has led to dramatic public showdowns between scientists and the panel’s chairman, Rep. John Dingell, a Michigan Democrat.
But these public hearings did not provide the same safeguards as court proceedings. At the Dingell hearings, the accused scientists could not confront their accusers and cross-examine them, or call their own witnesses. They had to submit their testimony ahead of time, and if Dingell or his staff didn’t like it, they could insist on changes—or the witness would suffer the consequences.
Dr. Bernadine Healy, the former director of the National Institutes of Health, said that when scientists come under Dingell’s scrutiny, they often are victimized by the subcommittee’s staff leaking damaging information about their cases to the media.
Some believe the investigative process is more harmful than the scientific misconduct it’s meant to correct. Science, by its nature, is self-correcting, they say.
“The notion of massive misconduct in science is really fairly ludicrousbecause of the inherent nature of science,” said Edward Richards, a University of Missouri law professor who has examined scientific misconduct. ”If your experiments don’t work, someone will find you out. There have been incidents of misconduct by scientists but, by and large, compared to any other part of the public sector, science is exemplary.”
Epilogue: Clinical trials
The fraud committed by Montreal surgeon Roger Poisson that triggered the Fisher investigation has done its greatest damage to clinical trials, a research tool that was largely pioneered by Fisher.
Clinical trials use the power of numbers—the statistical potency of comparing hundreds or thousands of patients—to determine whether a certain diagnostic test or diet or drug or surgical procedure is safe and effective.
Organizations around the country that conduct clinical trials have been deeply shaken by what happened to Fisher’s research group, the NationalSurgical Adjuvant Breast and Bowel Project. Some fear that federal officials’ efforts to deal with the scandal may end up causing more harm than good.
Last spring, shortly after the public revelation of the fraud at Poisson’s St. Luc’s Hospital in Montreal, National Cancer Institute officials moved quickly to establish tighter control over the clinical trials they funded.
Among the changes are a new department that will be a watchdog over clinical trials; surprise audits; more frequent routine audits; and a requirement that NCI be immediately notified of any evidence—no matter how small—of scientific misconduct.
You just can’t dismiss that in offhand fashion. Unfortunately, a bad thing happened and we’re going to pay a price. That means more cumbersome government regulations and a slight decrease in the number of centers, but I don’t see any other alternative.
Mace Rothenberg
Dr. Samuel Broder, the outgoing NCI director, told an NSABP conference in June that the tighter rules are the price scientists must pay for getting public money.
“No other nation in the world has been so committed to clinical trials, and the American taxpayers have a right to ask that we monitor and successfully administer such trials,” he told the group.
Dr. Bruce Chabner, director of NCI’s cancer treatment division, said the agency probably will double its budget for auditing patient records in clinical trials. Of course, he said, that means “you can do less research.” Every dollar spent on checking records is one that can’t be spent on recruiting patients.
Richard Peto, an internationally acclaimed statistician and co-director of the Oxford University Clinical Trial Service Unit in England, said the new NCI rules will make clinical trials harder to do.
“Because they make (studies) complicated, they make it impractical to make them large, and therefore they will be less reliable. You’ve got to get serious numbers into the trial. Otherwise the data will not be good, no matter how proper it is.”
Peto said the NSABP controversy has a “Kafka-esque” quality. “People who actually know about trials know that (Poisson’s falsifications) could not in principle have any material effect” on the studies’ outcomes, because he did not contribute enough patients to the trials to make a difference in the results.
NSABP “is being destroyed, all in the name of morality. The whole thing is completely hypocritical. They’ve destroyed research in the name of saving research.”
George Canellos, a former NCI official who is chief of medical oncology at the Dana-Farber Cancer Institute in Boston, also is worried about the new regulations.
Scientists will resist being second-guessed on each of their actions, he said.
“You have to basically trust that the vast majority of people do things honestly,” Canellos said. “The freedom of inquiry, the freedom to do your science is a very important part of scientific pursuit, and if you feel Big Daddy is watching you for everything, and if you are painted with the same brush as some of the cleverer cheaters, the demoralization to science will be awful.”
But Mace Rothenberg, a top official at the Southwest Oncological Group, which has conducted several clinical trials on cancer, took a different view.
“We’ve sustained a great trauma for clinical research that has shaken its foundations,” Rothenberg said. “You just can’t dismiss that in offhand fashion. Unfortunately, a bad thing happened and we’re going to pay a price. That means more cumbersome government regulations and a slight decrease in the number of centers, but I don’t see any other alternative.”
There is one new rule that troubled Rothenberg, though.
He didn’t like the requirement that study groups report the first sign of scientific misconduct.
“What does that mean?” Rothenberg said. “If you can’t locate a consent form, or if there’s an error in a date, must we notify the NCI immediately? I don’t think we can operate that way.”
Epilogue: NSABP
While other clinical trial groups fret, the atmosphere at the 500 member institutions of the NSABP is fearful.
With Fisher sidelined, they are uncertain about who will lead them into the future.
They also worry about the NSABP’s landmark breast cancer prevention trial, which was designed to test the anti-cancer drug tamoxifen on 16,000 healthy women to see whether it can prevent the disease.
That trial was put on hold after Fisher was fired, and only last month began accepting women again. Without the interruption, the study by now would have enrolled the total number needed to assess whether the drug works.
If the study shows tamoxifen is an effective deterrent of breast cancer, that delay could end up costing some women their lives.
Even if the breast cancer prevention trial gets back on track, it’s not clear whether NSABP will end up supervising it.
In fact, the organization’s future is uncertain.
In June, NCI Director Samuel Broder told NSABP members, “We must be sure that the NSABP succeeds and is restored to its proud reputation. We need to have the NSABP strong; we have other surgically oriented groups, but there are very few groups that have the tradition of the NSABP, so we want to work with you.”
Dr. Ronald Herberman, who was appointed by Pitt as NSABP’s interim chairman, also is upbeat. There’s a good possibility the organization will return to its previous strength, he said this month.
But in an interview last month with The Cancer Letter, a Washington, D.C.-based publication, Broder sent a different signal.
Asked whether the NSABP could survive “in its present form,” Broder said parts of it could, such as the prevention trial. But then he said the prevention trial could do very well without NSABP overseeing it.
Contributing to Broder’s ambivalence, perhaps, was NSABP’s selection of a successor to Fisher as chairman. Broder’s choice for the position was Dr. Janet Osuch, an outspoken breast cancer surgeon from Michigan State University who had roundly criticized Fisher for how he handled the Poisson scandal.
Instead, the NSABP executive committee chose Dr. Norman Wolmark, a respected breast cancer surgeon now at Allegheny General Hospital.
Broder, who last week announced he will leave the NCI in April, has not yet approved Wolmark’s selection.
The NCI director was clearly unhappy with the NSABP’s participation in Fisher’s lawsuit against Pitt, and said he would not approve Wolmark as long as the organization stayed in the lawsuit.
The NSABP’s executive committee still is suing Pitt, but has softened its demands.
While still insisting that the courts recognize their right to hire and fire their own chairman—which they believed was taken away from them when Fisher was deposed—the committee members decided this month to drop their demand that he be fully reinstated as head of the group.
If the leadership of the organization still is in question, so are many of its future studies.
One such trial wanted to test whether it was possible to eliminate surgery for some women suffering early breast cancers by giving women enough chemotherapy to shrink their breast tumors out of existence.
Fisher said another new study would have tested using the drug Taxol after surgery to determine if overall survival rates for breast cancer could be improved.
It’s uncertain if the NCI will ever approve them, he said.
Epilogue: St. Luc’s
At St. Luc’s Hospital, nearly three years after Poisson admitted falsifying patient records, about 300 women still come to be treated in a breast cancer study.
They subject themselves to mammograms twice a year, they take a placebo or tamoxifen and they allow information on their medical histories to be collected and kept.
What the women don’t know is that their participation may never be used to find better treatment for breast cancers.
Because of Poisson’s falsifications, NCI officials say data from all St. Luc’s patients should be thrown out of any past or future studies.
But NSABP officials argue that only the 99 past cases with proven falsifications by Poisson should be deleted.
Dr. Pierre-Michel Huet, St. Luc’s director of clinical research, is bothered that no one has told the women their contribution to science could be for naught.
“We are in a very bad position for that,” he said, but because he is getting conflicting signals from officials in Pittsburgh and Washington on whether the data will be used, he has chosen not to say anything to the women.
That is only one of the problems facing Huet, who took over as principal investigator for the St. Luc study after Poisson was ousted from it in 1991.
Because the hospital was suspended from the project after Poisson was removed, Huet inherited a study with hundreds of patients and no U.S. research money.
Another problem, he said, is Poisson, who refuses to give up his post at St. Luc’s.
“Once a doctor is affiliated with a hospital, it’s almost impossible under (Canadian) law to have him resign from the hospital unless there is very severe medical fault,” Huet explained.
Poisson, meanwhile, continues to be a passionate adherent of lumpectomies and the latest non-surgical treatments. His passion, after all, is what motivated him to fake the records in the first place, he said.
He believed the lumpectomy, which removes only the tumor and a small amount of tissue surrounding it, was the right treatment for most patients and that NSABP’s landmark 1985 study would prove it and persuade more doctors to use it. If getting to that point meant subjecting some women in the trial to mastectomies in order to have a comparison group, it was worth it.
Later on, he said, he changed records so women would be eligible for tamoxifen and other experimental drugs, which they would not have been able to obtain otherwise.
Huet said he thinks Poisson genuinely believes he acted in his patients’ best interests, but he does not defend him.
“You are not allowed to put in danger all the study because you think you’re right. It’s gambling, and you are not allowed to gamble when thousands of women are enrolled and millions of dollars are involved.”
Dr. Richard Margolese of Montreal’s Jewish General Hospital, who is a member of NSABP’s executive committee and has known Poisson for years, is equally critical.
“We all had the problems (Poisson) had. We all wanted to include more cases than we did. But none of us did what he did.”
Epilogue: The activists
In recent years, the number of groups advocating better breast cancer treatment has proliferated.
As the Fisher controversy drags on, these activists are unified in their criticism of Poisson’s fraud.
But they are sharply divided on another issue—the ethics of Fisher’s breast cancer prevention trial, which gives healthy women tamoxifen. While Fisher believes tamoxifen may prevent breast cancer, it also increases the risk of uterine cancer.
Those already opposed to the idea of such an experiment were outraged when they learned from news stories in February that Fisher had delayed divulging that several patients in an earlier tamoxifen study had died after developing uterine cancer.
To opponents of the study, Fisher’s actions were a scandal far worse than the falsified records in Montreal.
“As far as I’m concerned, they fired the right guy for the wrong reason,” said Nancy Evans of San Francisco’s Breast Cancer Action.
Fisher said he resisted releasing the information because he believed the deaths needed to be investigated more fully.
To this day, he thinks people like Evans have overreacted to the news of uterine cancer deaths.
Of the six women in the previous study who died after getting uterine cancer, records show, only five had taken tamoxifen, and only one of the five had died from a malignancy that was clearly linked to uterine cancer.
“The important issue here is whether a woman who had breast cancer and received tamoxifen died with uterine cancer or from uterine cancer,” Fisher said. “This is a very difficult call for physicians, pathologists and oncologists to make … and such medical detective work takes a long time.”
Some other breast cancer advocates side with Fisher. Amy Langer at the National Association of Breast Cancer Organizations said the tamoxifen trial is worthwhile because “we currently have no prevention methods.”
As the tamoxifen study resumed last month, though, activists such as Evans were working to alert women to the drug’s dangers in hopes they would not participate.
Epilogue: Lumpectomies
From the moment the Montreal fraud was discovered, the most critical question was: Did the falsifications undermine the 1985 study showing that lumpectomies were as effective as more disfiguring mastectomies?
The most definitive answer came in mid-November when the NCI announced the results of an intensive re-examination of the study.
It found that Fisher was right all along—Poisson’s falsifications hadn’t made any difference in the study’s conclusions.
It also is improbable that Poisson’s fraud affected any other NSABP studies.
Poisson had tampered with 99 patients’ records, spread among 14 studies that looked at everything from alternative methods of surgery to different combinations of chemotherapy.
The lumpectomy study included only six falsified records, representing three-tenths of a percent of the 2,163 women who participated.
Of Poisson’s 93 other patients with falsified records, the largest number—35—were in a study looking at the effectiveness of tamoxifen in preventing a recurrence of breast cancer. They represented 1 percent of the 2,892 women in the project.
Fisher said that the NCI’s audit, bolstered by a study of lumpectomies released last month by the General Accounting Office, amounted to “a 100 percent vindication” of his stewardship of NSABP.
But NCI Director Broder, whose agency spent about $2 million on its investigation of Fisher’s group, disagreed. The fact that the study results remained the same did not absolve NSABP of its weaknesses in checking patient records or its slowness in publishing a scientific article explaining the effects of fraudulent data.
“That’s like saying it’s OK to go 100 miles an hour through a residential neighborhood as long as you don’t hit anybody.”
Epilogue: The players
Since March, when Fisher was fired, the political landscape in Washington and Pittsburgh has shifted dramatically.
Rep. Dingell has lost much of the power he had to police scientific misconduct. The Republican sweep last month stripped him of his chairmanship and sent his investigative staff looking for new jobs.
Broder plans to leave the NCI in April and join a Florida pharmaceutical company. Although Broder took plenty of heat from all sides for his actions during the Fisher episode, he is unapologetic, and says it did not play a direct role in his decision to leave.
Broder’s top deputy, Bruce Chabner, the man who oversees NCI’s cancer treatment programs, also will leave the agency next spring for a position at Massachusetts General Hospital.
Michael Friedman, the NCI official who made the phone call to fire Fisher at the request of his supervisors, said he also is considering leaving the institute, after a 22-year career there.
He said he still believes that the NSABP’s administrative problems were ”of unprecedented scope and seriousness.”
But does Friedman think that Fisher should have been fired?
“There certainly could have been better ways that some aspects of this could have been handled,” he said slowly, then added, “I have not yet had the opportunity for dispassionate reflection on that matter.”
Neither Friedman nor any other NCI official has talked with Fisher since he was fired.
Perhaps most galling for Fisher has been his shunning by the NCI’s Broder.
After his wife contracted breast cancer, Broder called Fisher last December for advice. They had long, friendly telephone conversations before the scandal became public, Fisher said.
Fisher tried to call Broder to set up a meeting in the weeks after the news broke in March, but said he never got through to him and never received a call back.
Epilogue: Bernard Fisher
In the case of Dr. Bernard Fisher, the facts are these:


- He never was accused of falsifying information about patients himself.
- The fraud committed by Poisson on 99 patients’ records has not changed the basic outcome of the studies he directed at NSABP.
- There is no evidence of systematic fraud in the other medical centers Fisher oversaw.
Yet, in the end, Fisher lost his career, and what may have been lifesaving research has been derailed or at least delayed.
Fisher clearly had his faults. He had little patience for what he derisively called “BAPs”—bureaucrats, administrators and politicians—the very people he had to answer to in order to continue his federally funded research.
Also, he was slow to reveal bad news, believing that he knew best when the public should find out about such issues as the falsifications and the uterine cancer cases.
It is part of his basic personality, said one longtime friend.
“Bernie is a bit of a pat-you-on-the-head sort,” said Helene Brown, a health educator at UCLA. “And when people ask, ‘Why didn’t you take steps to tell the whole world?’ (about the Canadian fraud), the bottom line is that the study didn’t change, and inside, he felt, as long as it didn’t change, I’m not going to upset all these women.”
He has paid a steep price for that attitude.
He knows that his name might always be associated with “l’affaire Poisson”—the scandal in Montreal.
He desperately wants his reputation restored.
That is why he spends each day writing down “the truth” about what really happened.
He doesn’t know when his story will get to be told, but he writes it down anyway, hoping that “someday, somebody, somewhere will hear it.”
Mackenzie Carpenter, was a projects writer for the Post-Gazette. The Princeton, N.J., native previously worked for United Press International, and for public television in both Washington D.C. and Harrisburg. She received a B.A. from Trinity College in Hartford, Conn., and a master’s degree in legal studies from Yale Law School. She is retired and living in Pittsburgh.
Steve Twedt, was a medical writer for the Post-Gazette. A native of Portland, Ore., Twedt has worked for the newspaper since 1993. Before that, he worked for The Pittsburgh Press and for newspapers in Washington, Oregon and Alaska. Twedt earned a bachelor’s degree from the University of Oregon. He covers business, finance, health and national news at the Post-Gazette.
Copyright ©, Pittsburgh Post-Gazette, 2019, all rights reserved. Reprinted with permission.