Keytruda was approved by FDA as monotherapy for the treatment of adult and pediatric patients with unresectable or metastatic tumor mutational burden-high (TMB-H) [≥10 mutations/megabase (mut/Mb)] solid tumors, as determined by an FDA-approved test, that have progressed following prior treatment and who have no satisfactory alternative treatment options.
This indication is approved under accelerated approval based on tumor response rate and durability of response. Continued approval for this indication may be contingent upon verification and description of clinical benefit in the confirmatory trials. The safety and effectiveness of Keytruda in pediatric patients with TMB-H central nervous system cancers have not been established.
FDA also approved the FoundationOne CDx test as the companion diagnostic to identify patients with solid tumors that are TMB-H (≥10 mutations/ megabase) who may benefit from immunotherapy treatment with KEYTRUDA monotherapy.
“These approvals stem from years of research into how TMB levels may influence a patient’s response to immunotherapy,” Brian Alexander, chief medical officer of Foundation Medicine said in a statement. “It’s critical that healthcare professionals have access to a validated genomic test to measure TMB in clinical tumor assessments and pinpoint those who are more likely to respond. We’re proud to be collaborating with Merck to help match appropriate patients to this important treatment.”
The accelerated approval was based on data from a prospectively-planned retrospective analysis of 10 cohorts (A through J) of patients with various previously treated unresectable or metastatic solid tumors with TMB-H, who were enrolled in KEYNOTE-158 (NCT02628067), a multicenter, non-randomized, open-label trial evaluating KEYTRUDA (200 mg every three weeks).
The trial excluded patients who previously received an anti-PD-1 or other immune-modulating monoclonal antibody, or who had an autoimmune disease, or a medical condition that required immunosuppression. TMB status was assessed using the FoundationOne CDx assay and pre-specified cutpoints of ≥10 and ≥13 mut/Mb, and testing was blinded with respect to clinical outcomes. Tumor response was assessed every nine weeks for the first 12 months and every 12 weeks thereafter. The major efficacy outcome measures were objective response rate (ORR) and duration of response (DOR) in the patients who received at least one dose of KEYTRUDA as assessed by blinded independent central review (BICR) according to Response Evaluation Criteria in Solid Tumors (RECIST) v1.1, modified to follow a maximum of 10 target lesions and a maximum of five target lesions per organ.
In KEYNOTE-158, 1,050 patients were included in the efficacy analysis population. TMB was analyzed in the subset of 790 patients with sufficient tissue for testing based on protocol-specified testing requirements. Of the 790 patients, 102 (13%) had tumors identified as TMB-H, defined as TMB ≥10 mut/Mb. The study population characteristics of these 102 patients were: median age of 61 years (range, 27 to 80); 34% age 65 or older; 34% male; 81% White; and 41% Eastern Cooperative Oncology Group (ECOG) Performance Status (PS) of 0 and 58% ECOG PS of 1. Fifty-six percent of patients had at least two prior lines of therapy.
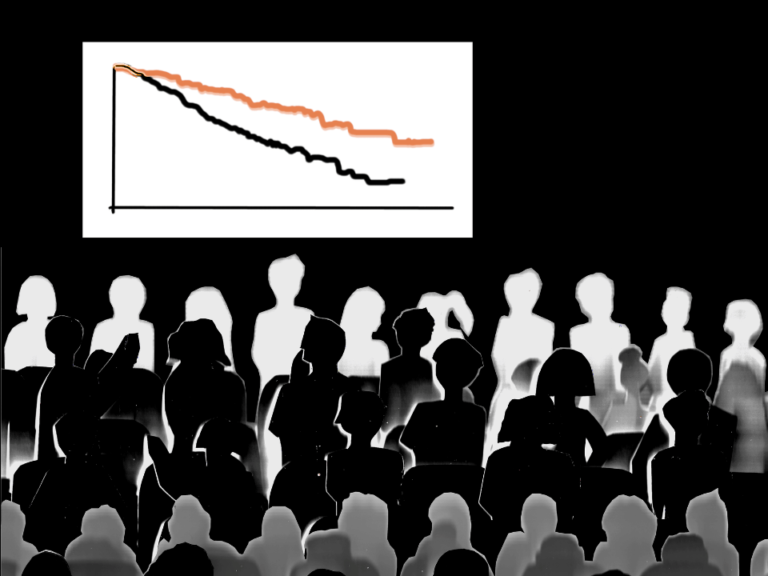
In the 102 patients whose tumors were TMB-H, KEYTRUDA demonstrated an ORR of 29% (95% CI, 21-39), with a complete response rate of 4% and a partial response rate of 25%. After a median follow-up time of 11.1 months, the median DOR had not been reached (range, 2.2+ to 34.8+ months). Among the 30 responding patients, 57% had ongoing responses of 12 months or longer, and 50% had ongoing responses of 24 months or longer.
In a pre-specified analysis of patients with TMB ≥13 mut/Mb (n=70), KEYTRUDA demonstrated an ORR of 37% (95% CI, 26-50), with a complete response rate of 3% and a partial response rate of 34%. After a median follow-up time of 11.1 months, the median DOR had not been reached (range, 2.2+ to 34.8+ months). Among the 26 responding patients, 58% had ongoing responses of 12 months or longer, and 50% had ongoing responses of 24 months or longer. In an exploratory analysis in 32 patients whose cancer had TMB ≥10 mut/Mb and <13 mut/Mb, the ORR was 13% (95% CI, 4-29), including two complete responses and two partial responses.