This story is part of The Cancer Letter’s ongoing coverage of COVID-19’s impact on oncology. A full list of our coverage, as well as the latest meeting cancellations, is available here.
Nicole Kuderer and colleagues are to be congratulated for their report—in The Lancet and at the ASCO 2020 Annual Meeting—on the impact of COVID-19 on a cohort of patients with cancer.
In a very short time, these researchers used social media and novel ways of communicating to bring together healthcare providers from over 100 institutions in the US, Canada, and Europe to form the COVID-19 and Cancer Consortium (CCC19) database.
This group is actively collecting data, and this publication represents an initial study of outcomes in cancer patients infected with SARS-CoV-2. It is an observational study, with all the caveats of an observational study, but it is data. It provides fact and understanding of the disease in cancer patients. It allows the medical community to change our practices for the betterment of patients during the pandemic.
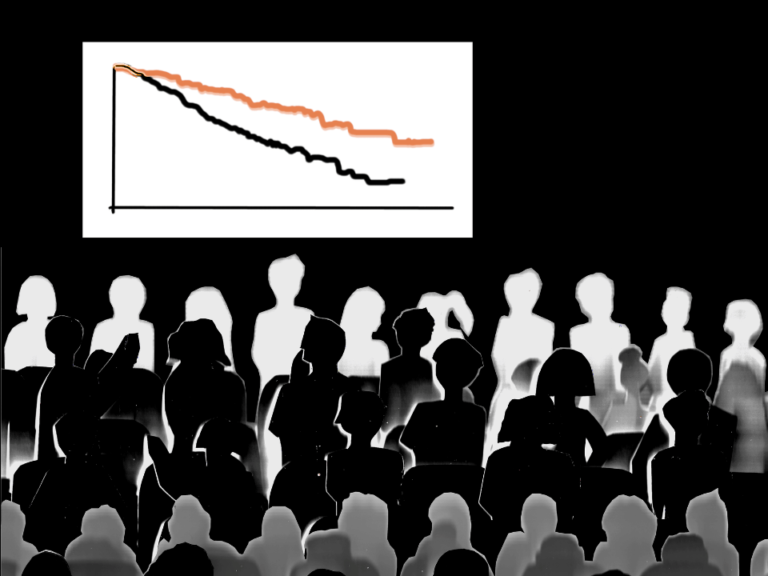
We already know that studies show that SARS-CoV-2-infected older persons with comorbid diseases, especially diabetes, lung and cardiovascular disease are at higher risk of poor outcomes. This study shows that patients with active cancer or progressing cancer have a higher risk of death after contracting the SARS-CoV-2, compared to the general population with the infection.
Most importantly, this study suggests that that elective surgery does not put patients at increased risk of adverse outcomes if infected postoperatively. It also suggests that cancer treatment with non-cytotoxic chemotherapy, and maintenance chemotherapy can continue with caution during the pandemic. It does support frequent testing for SAR-CoV-2 infection in those receiving cancer treatment.
It is known that there are risks associated with “gun-slinger medicine.” This paper is now one of several studies to suggest that use of these drugs, especially in combination, is associated with increased risk of death.
Future analysis of the cohort will likely yield more information on risk of specific cancers or risk following myelosuppression associated with cytotoxic chemotherapy or immune activation associated with immunotherapy.
A most disturbing finding is that 40% of the 928 (371) patients in the cohort, were taking hydroxychloroquine, azithromycin, or both, and only two did so while enrolled on a clinical trial of these drugs. While we cannot assume an exact proportion, this finding means a lot of people with SARS-CoV-2 are taking these medicines. It speaks volumes to societal failure to appreciate the importance of using the scientific method to guide the practice of medicine.
There are some who say that desperate patients have the “right to try” a medicine that might help. Fact is, the data to support efficacy of these drugs to treat or prevent COVID-19 infection is pitifully poor. Indeed, the theory on why it would work is weak. In February, March, and April of this year, one could just barely justify a clinical trial to establish efficacy, but taking these drugs outside of a well-designed clinical trial was and is appalling.
It is known that there are risks associated with “gun-slinger medicine.” This paper is now one of several studies to suggest that use of these drugs, especially in combination, is associated with increased risk of death.
I am less critical of the patients taking these drugs. They are afraid and desperate. I am outraged at the “so-called” doctors who prescribe these treatments. They ought to know better. Every patient prescribed these drugs is an experiment: each one is a “guinea pig” in a poorly designed clinical trial of one subject. Failure to support the science-based practice of medicine and the conduct of clinical trials slows progress in figuring out how to best treat our patients.
This paper and its publication provide an example of the best of medicine and the worst of medicine. The healthcare providers who prescribe medicines without scientific basis are doing the exact opposite of those physicians and scientists who formed the COVID-19 and Cancer Consortium database.