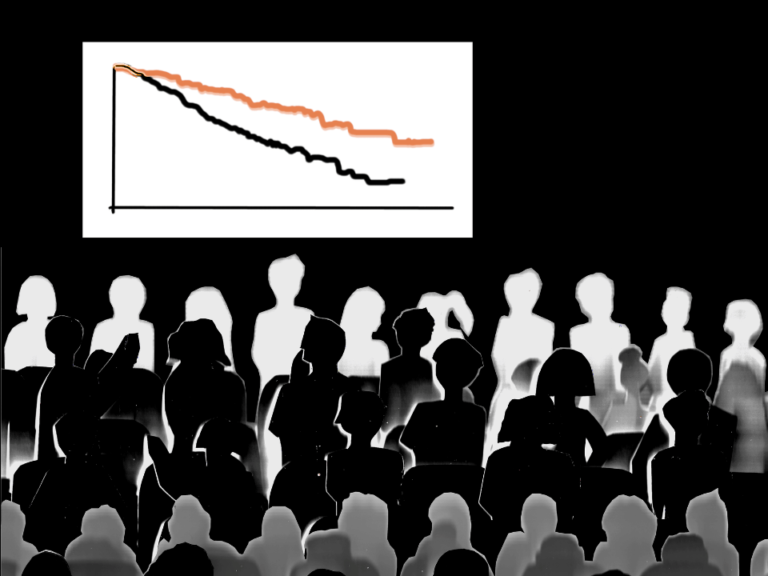
Keytruda in combination with chemotherapy for the first-line treatment of patients with advanced or metastatic urothelial carcinoma did not meet its pre-specified dual primary endpoints of overall survival or progression-free survival, compared with standard of care chemotherapy.
Keytruda is sponsored by Merck.
In the final analysis of the study, there was an improvement in OS and PFS for patients treated with Keytruda in combination with chemotherapy (cisplatin or carboplatin plus gemcitabine) compared to chemotherapy alone; however, these results did not meet statistical significance per the pre-specified statistical plan.
The monotherapy arm of the study was not formally tested, since superiority was not reached for OS or PFS in the Keytruda combination arm. The safety profile of Keytruda in this trial was consistent with previously reported studies, and no new safety signals were identified.
Keytruda has three FDA-approved bladder cancer indications across multiple types and stages of bladder cancer. Additionally, Merck has an extensive clinical development program in bladder cancer and is continuing to evaluate Keytruda as monotherapy and in combination with other anti-cancer therapies across several disease settings (i.e., metastatic, muscle invasive bladder cancer, and non-muscle invasive bladder cancer).