The Cancer Letter spoke with leaders at Seattle Cancer Care Alliance/Fred Hutchinson Cancer Research Center MD Anderson Cancer Center, University of California, Los Angeles, and Robert H. Lurie Comprehensive Cancer Center of Northwestern University to gauge the impact of coronavirus.
“We don’t want to be alarmist, but we do want to be truthful. The truth is that all cancer patients should be concerned about COVID-19 because they are at higher risk,” said Steve Pergam, medical director of Infection Prevention at Seattle Cancer Care Alliance and clinical and infectious disease researcher at Fred Hutch, which does not provide patient care on its campus. “We are taking numerous precautions, such as screening all patients, staff and providers for respiratory symptoms (including runny nose, congestion, fever or shortness of breath) upon arrival at the clinic.”
Washington has 420 confirmed cases of COVID-19 and 31 deaths—the highest of any state.
“With a virus that is unpredictable and rapidly changing, we must do everything we can to keep our patients safe,” said Peter WT Pisters, president of MD Anderson Cancer Center. “We also have a responsibility to advise on other proactive measures that can be taken at a community level to slow down the spread of the disease within our community and across the nation.”
Even now, patients are worried about coming in for their regular clinical care.
“We hear concerns from patients, and we are working hard to minimize their time spent in hospital facilities,” Leonidas C. Platanias, director of Northwestern’s Robert H. Lurie Comprehensive Cancer Center, said to The Cancer Letter. “We are being proactive and have in place new procedures specifically addressing COVID-19 issues. For instance, patients calling for an appointment are being screened for fever, cough and recent international travel.”
Patients at Lurie Comprehensive Cancer Center are screened for coronavirus prior to their appointment. There’s a COVID-19 nurse hotline, and a specific COVID-19 response team.
Illinois has 25 confirmed COVID-19 cases and no deaths.
“Our caregivers are being asked to remain vigilant with infectious disease protocols—evaluate symptoms, take travel history, and contact the emerging infectious disease team regarding any potential COVID-19 cases,” a spokesperson for UCLA Health said to The Cancer Letter. “If a patient meets criteria for testing established by the CDC, biological samples are taken to determine an accurate diagnosis.”
California, has more than 200 cases and four deaths.
“Staff caring for patients suspected of carrying any contagious disease take all appropriate precautions to contain transmission,” the UCLA spokesperson said. “Our overriding priority at all times is to provide high-quality patient care while ensuring employee safety at all UCLA Health hospitals and clinics.”
Cancer center leaders spoke with Alexandria Carolan, a reporter with The Cancer Letter.
Alexandria Carolan: How are cancer patients affected by this outbreak? Are they disproportionately at risk because they require more consistent care?
Steve Pergam (Seattle Cancer Care Alliance/Fred Hutch): We don’t want to be alarmist, but we do want to be truthful. The truth is that all cancer patients should be concerned about COVID-19 because they are at higher risk. Bone marrow transplant patients and those with blood malignancies such as non-Hodgkin lymphoma, chronic lymphocytic leukemia, acute myeloid leukemia, acute lymphoblastic leukemia and multiple myeloma are at even greater risk because their immune systems are most compromised. Any cancer patient in active treatment—this includes surgery, radiation, chemotherapy and/or immunotherapy—is also considered high-risk. And cancer patients who are over 70 face an elevated risk due to their age.
Peter WT Pisters (MD Anderson): Ensuring the safety of our patients and the health of our workforce members remains our highest priorities during this pandemic. Research shows that patients currently receiving cancer treatment, cancer survivors, older patients, and those with weakened immune systems or serious medical conditions are uniquely vulnerable to the 2019 novel coronavirus disease (COVID-19). Because of these factors, we have an even greater obligation to implement proactive efforts that go above and beyond CDC guidelines in order to protect our patients and employees.
Leonidas Platanias (Lurie Comprehensive Cancer Center): Many of our patients with cancer are at higher risk in terms of morbidity and mortality than the general population due to the treatments they receive, including chemotherapy and radiation therapy. Patients with hematological malignancies who receive intensive chemotherapy or patients undergoing stem cell transplant are particularly high-risk groups. In addition, patients undergoing cancer treatment are at higher risk for exposure to the virus because they have to travel to and from the facility to get their care, interact with a large team of healthcare providers when on-site, and visit facilities where patients with COVID-19 are also receiving care.
How do you communicate with cancer patients about this outbreak?
SP: It is our job to be open and transparent with our patients about COVID-19 and the impact it has on our patient community. At Seattle Cancer Care Alliance, we have a dedicated webpage, which has become a repository of patient-facing communications. There patients will find our most up-to-date information related to COVID-19 and the measures we’re taking to ensure the health and safety of our patient community. We have protocols and systems in place to keep all patients, visitors and healthcare workers safe. We have also established a nurse triage line for patients to call with their COVID-19-related concerns. We are asking patients to call that line in advance of their appointments if they are experiencing symptoms related to the virus. Our trained nurses will provide guidance about whether the patient needs to reschedule or cancel their appointment.
PP: As an institution, we are committed to providing frequent and transparent communications so that our patients and workforce members have up-to-date, factual information about this rapidly evolving outbreak. A dedicated page on our external website explains the proactive measures MD Anderson is taking to prevent the introduction or spread of COVID-19 at any of our campuses. These same messages are shared across MD Anderson’s social media channels and my own Twitter account (@ppisters), through patient portal notices directly to patients, and with our care teams and staff through daily emails and alerts.
At MD Anderson, we believe communication is everyone’s responsibility, and I take my role as “Communicator in Chief” seriously. With information evolving daily, it is important to separate facts from fear. I have started a series of short videos, available on MD Anderson’s YouTube channel, to inform all of our stakeholders about MD Anderson’s plans to protect our patients, workforce and community. Key precautions, including enhanced screening protocols and visitor limitations, also are highlighted in multiple languages on signage throughout our campuses.
LP: We have a website specifically dedicated to providing COVID-19 information and answers to frequently asked questions. We have also set up a COVID-19 hotline. Of course, our physicians and nurses also spend time with our patients and their families directly addressing their questions.
Have patients expressed concerns about coming in, because they don’t want to be exposed to the virus?
SP: We have had patients express their concerns and, as always, planning and preparedness are essential to maintaining our high levels of care as we navigate this pandemic. Seattle Cancer Care Alliance has an extensive infection prevention protocol in place to prevent the spread of illness among patients and staff. We are taking numerous precautions, such as screening all patients, staff and providers for respiratory symptoms (including runny nose, congestion, fever or shortness of breath) upon arrival at the clinic. We are also continuing routine cleaning of high-touch surfaces such as door handles and elevator buttons and using disinfectants that are effective at killing COVID-19. We have a responsibility to the community to continue to provide top-notch cancer care, and we take that responsibility very seriously.
PP: Many patients and their caregivers have questions and concerns about COVID-19, including questions about the risk of travel. We understand these concerns and recommend patients follow the advice of their care teams and guidance from CDC. We ask that patients who need to fly to Houston contact their care team first. We are making recommendations on a patient-by-patient basis, considering treatment timeline, type of treatment or appointment, patient age, other health conditions and any current symptoms or side effects. We are also encouraging everyone to take everyday preventive actions to stop the spread of respiratory infections by washing their hands often for at least 20 seconds, avoiding touching their face and reconsidering participation at crowded events.
LP: Yes, we hear concerns from patients, and we are working hard to minimize their time spent in hospital facilities. To minimize potential COVID-19 exposure, we are being proactive and have in place new procedures specifically addressing COVD-19 issues. For instance, patients calling for an appointment are being screened for fever, cough and recent international travel. Depending on the answers to the screening questions, they are being triaged to a COVID-19 nurse hotline or are scheduled for their visit with instructions to wear a mask and take other precautions, if necessary. We also have established a COVID-19 response team that is activated if any patient arrives after failing the screening questions. In this case, the patient and their companions are given masks and brought to the closest negative airflow room for further assessment. We work closely with the Northwestern Medicine Infection Prevention team on these measures.
Does leadership foresee a surge of patients coming in for emergency care and taking up beds, potentially even disrupting the regular care of cancer patients?
SP: As an outpatient clinic, Seattle Cancer Care Alliance is not equipped to serve patients who need emergency care. This is a fluid, everchanging situation and our leadership has certainly had discussions about the potential for this. That said, we are operating as normally as possible and continuing to care for those patients who are in active treatment.


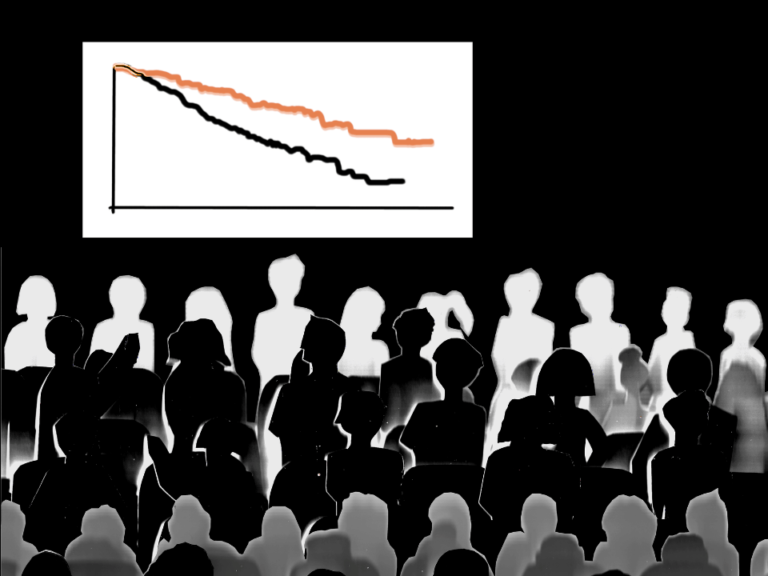
PP: We know health care systems that put diligent protective measures in place early in the course of an epidemic are more successful in containing infection and ensuring that the system has the capacity to serve patients if severe cases arise. In public health, this concept is known as “flattening the curve” (see graph). We actively are collaborating with health systems leaders in our region as well as city, county and state officials to take proactive measures now to help protect against a scenario where regular care is disrupted.
LP: Yes, we expect a surge of patients and are working closely with others across the health system to develop contingency plans designed to minimize any impact on patients who need cancer treatment. We have particular concern about the availability of ICU beds and respirators that may be needed. This is important, because if the system is overwhelmed, it will affect patients who need intensive care management for cancer. Plans are being developed and space identified for additional respirators and intensive care equipment if necessary in the near future.
Are there concerns about disruptions to drug supply?
SP: Drug shortages have not been a serious concern for our organization yet. Our main concern now is maintaining a reliable supply of cleaning products, masks and other personal protective equipment, all of which are key to prevent the spread of the virus among our patients and staff.
Our leadership is also paying close attention to blood supplies. As people adopt social distancing practices, we are noticing a drop in blood donations. We are encouraging people who can to donate blood so we can avoid a shortage.
PP: Our leadership team is proactively working to ensure we have the necessary supplies, equipment and training in place to prevent the spread of infection and to continue patient care without interruption. We are monitoring the situation closely and are not currently concerned about disruptions to the drug supply.
LP: Yes, there are concerns, especially as a significant number of drugs come from China. For instance, 80% of the U.S. antibiotic supply is made in China, and there may be disruptions because of the intensity of COVID-19 there. Working closely with the Northwestern Medicine health system and our hospital pharmacy, we have a plan in place to ensure that all important medications for the treatment of cancer will continue to be available.
Has your cancer center updated its staff and faculty policies because of coronavirus? I mean, for travel, work from home, etc.
SP: Seattle Cancer Care Alliance has had to make the very difficult decision to reschedule non-essential patient visits for the time being out of concern for our patients’ health—and to make sure that we are well-positioned to care for our patients in active treatment and prepare as the number of COVID-19 cases in our area continues to grow.
PP: MD Anderson already has restrictions in place for all employee business travel, domestic and international, through April 29. We have also asked employees to refrain from personal travel to areas with a Level 2 and Level 3 travel advisory based on federal guidelines. As an additional precaution, our Information Security team developed a COVID-19 Travel Registry (CTR) aimed at preventing the introduction or spread of the novel coronavirus at any of our campuses. With the CTR, employees have the opportunity to share details of recent personal travel, as well as the travel of their household members, with our Office of Employee Health and Wellbeing. All of the information is confidential.
Additionally, we have empowered and encouraged our workforce to utilize Skype, WebEx and other remote participation tools to conduct meetings, when possible. These technologies still allow for engaging discussion during events like institutional and external grand rounds, as I experienced firsthand when leading a virtual lecture with Harvard School of Public Health this week. In the near future, some employees will be asked to work from home and some will be redeployed to help carry out operations on campus. We have chosen to go above and beyond CDC-recommended guidelines from the beginning and we will continue to closely monitor this pandemic.
We don’t want to be alarmist, but we do want to be truthful. The truth is that all cancer patients should be concerned about COVID-19 because they are at higher risk.
Steve Pergam
LP: Yes. All business travel outside of our state is banned by Northwestern Medicine, and we advise our faculty and staff to minimize their personal travel as well. We have also cancelled all Cancer Center seminars and grand rounds. Yesterday, we announced that the monthly meetings for the different Cancer Center Support Grant programs will no longer take place in person; we will be conducting them online, via teleconference. These precautions will be in place for the next two months, and we will reassess the situation then. In general, we have been promoting social distancing, and have asked our faculty and staff to minimize unnecessary in-person meetings. We are also in the process of defining a policy regarding interactions with vendors visiting us and the ability for our staff to work off-site.
How does your cancer center anticipate responding to COVID-19 if the outbreak continues to worsen?
SP: Currently, our focus is on taking care of patients in active treatment while also being incredibly vigilant about preventing the spread of COVID-19 among our patient and staff community. Our infection prevention team is having ongoing discussions with leadership and our state and local public health officials in anticipation of the outbreak worsening. We are continually adapting as the situation evolves. We communicate with our patients about any changes to our policies and operations via the COVID-19 webpage on the SCCA website.
PP: With a virus that is unpredictable and rapidly changing, we must do everything we can to keep our patients safe. We also have a responsibility to advise on other proactive measures that can be taken at a community level to slow down the spread of the disease within our community and across the nation. We are collaborating with other institutions in our region and working with city, county and state health officials to monitor updates, develop community screening protocols and expand access to testing.
Our emergency plan includes detailed actions for outbreaks like COVID-19. We are prepared to take additional steps to ensure the safety of our patients as the situation progresses. MD Anderson began limiting visitors and expanded screening on campus the first week of March. Starting March 13, patient visitors (already limited to two people who are not showing symptoms) must be age 18 or older.
Throughout all of this, we strive to keep in mind our core value of Caring, using our expertise and best judgement to allow for compassionate exceptions on a case-by-case basis. Visitors who are not caregivers and who do not have mission-critical business with MD Anderson are restricted from campus. All volunteer shifts have been canceled as a significant portion of our volunteer population are cancer survivors or elderly adults at greater risk. Going forward, employees, patients and caregivers will only have access to limited entry points on our campuses.
Our testing capacity for COVID-19 is currently reserved for patients as testing kits remain in high demand. However, we are dedicated to providing a pathway for employee testing as well. We are preparing one of our Houston-area diagnostic imaging clinics to become a future testing site for MD Anderson patients and employees. I am inspired by the way the MD Anderson community has come together to protect the patients we serve. We will continue to provide clear and consistent communication to all stakeholders as we implement additional measures to mitigate the impact of the COVID-19 pandemic.
LP: We have been working closely with Northwestern Medicine to optimize and update plans as needed. We will intensify the measures mentioned above and we will consider further escalations as needed. The next step will be to have all of our staff working remotely. For now, we don’t plan to suspend the research operations of our labs, but this may be something that we may have to face in the future. Our priority is the safety and the well-being of our patients.
This story is part of The Cancer Letter’s ongoing coverage of COVID-19’s impact on oncology. A full list of our coverage, as well as the latest meeting cancellations, is available here.