This story is part of The Cancer Letter’s ongoing coverage of COVID-19’s impact on oncology. A full list of our coverage is available here.
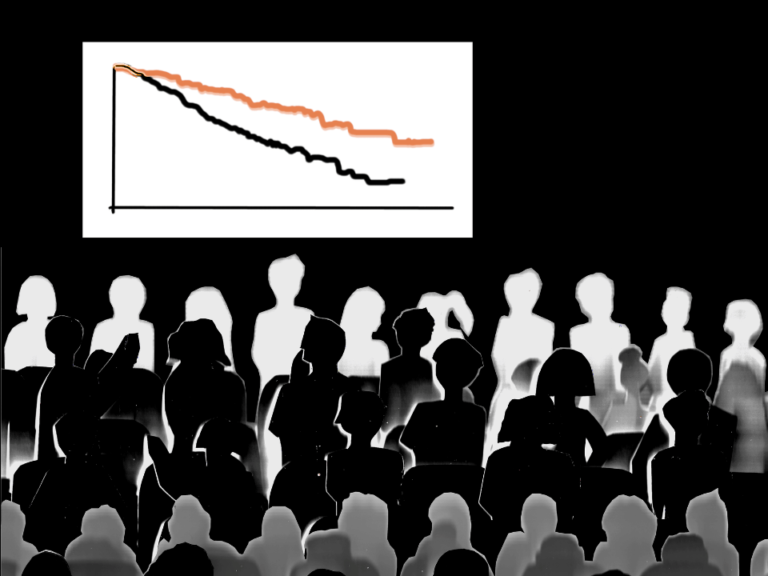
This January, the American Cancer Society reported the sharpest drop in U.S. cancer mortality ever recorded. Between 2016 and 2017, the death rate from cancer fell 2.2%, continuing the trajectory of a 29% decline in cancer mortality since 1991.
Within a month after ACS reported those numbers, the COVID-19 pandemic hit, sending shockwaves through the already fragmented U.S. healthcare system. The pandemic could potentially reverse a decades-long downward trend in cancer mortality. We must not let this happen.
Specifically, we must ensure patients can get indicated screenings they need to detect cancer early, prevent it when possible, and save lives. We must also make sure that cancer patients continue their treatment regimens already underway uninterrupted and initiate new treatment for cancer when needed.
We have our work cut out for us—patients are understandably worried about seeking care during the pandemic, which has caused the death of nearly 200,000 people in the U.S., and continues to claim the lives of around 1,000 people in the country every day. These numbers do not adequately reflect the collective trauma and depth of our loss.
As we continue to mourn the lives lost due to the pandemic and adapt our lives to the measures necessary to keep one another safe, we must recommit to lifesaving preventive measures such as screening for cancer. Every year, cancer kills 600,000 people in the U.S. These lives, too, are invaluable. The risk of a significant reduction in screenings, a proven method to reduce mortality from cancer, is too great to bear.
Any significant drop in screenings could have profound consequences. Routine colonoscopies that led to the removal of noncancerous colorectal polyps reduced mortality from colorectal cancer by 50%, according to a study published in the New England Journal of Medicine.
Screening exams also enable health care providers to detect and treat malignancies early, when they are often more responsive to therapy. A study published in the journal Cancer found that routine mammograms reduced a woman’s risk of dying from breast cancer within 10 years of her diagnosis by 41%, and also led to a 25% reduction in being diagnosed with advanced breast cancer, which is much more difficult to treat.
According to a 2016 study published in the British Journal of Cancer, screening for cervical cancer has prevented nearly 68% of would-be deaths from the disease.
To gain the lifesaving benefits of routine screening, we must safely resume scheduling patients for these exams—or risk a worse outcome in some individuals.
How we got here
As the pandemic peaked in waves around the country, healthcare organizations and local officials released policies to delay elective procedures. For many, “elective procedures” included routine screening exams. These measures were necessary for providers to assess the threat of COVID-19, or for hospitals with active COVID-19 wards to redirect staff and resources towards virus-infected patients.
Now, patients continue to delay preventive screenings for many reasons. At first, patients were told to postpone screenings by their healthcare providers, so they did. But even as hospitals have developed protocols to deliver routine care in a much safer environment, screening rates remain too low, and ultimately bad outcomes could result in lives lost.
Again, this is understandable. Even in the best of times, we are not capitalizing on the full potential of prevention measures that we know work. As of 2015, screenings for breast, cervical and colon cancer fell short of targets set by the Office of Disease Prevention and Health Promotion.
These, of course, are not the best of times. The pandemic temporarily brought routine screenings to a halt. That type of inertia is dangerous, especially as the pandemic intensifies factors that make barriers to care worse. Patients tend to seek less care in an economic downturn—they conserve their health care dollars for acute issues and emergencies.
Patients across the world are now suffering from economic hardship. The World Bank predicts the global economy will shrink by 5.2% this year, and that the U.S. economy will contract by 6.1%. Moreover, up to 12 million Americans may have lost their employer-sponsored health insurance during the pandemic, according to the Economic Policy Institute, adding to people’s financial stress.
Besides the economic hardship triggered by the pandemic, patients are sometimes afraid. The background noise of COVID-19 can drown out other health concerns. With a lack of clear direction and/or conflicting messages, some patients have been receiving inconsistent information about how and when to resume health care services.
With state and local healthcare leaders overburdened with the requirements of the pandemic response, it leaves few stakeholders to bang the drum about the importance of screening for cancer—and cancer screening is needed to maintain the health and wellbeing of individuals in the U.S., the healthcare system, and the country as a whole.
What we risk if we fail
Already, COVID-19 has halted cancer screenings to a degree that could negatively affect outcomes. Researchers estimate that mammograms, a crucial tool for early detection of breast cancer, have dropped anywhere from 75% to 95% since March 2020. Pandemic-related screening delays could cause an excess of 10,000 deaths over the next 10 years, National Cancer Institute director Ned Sharpless told STAT this past June—resulting in a 1% increase in expected deaths for the decade.
As of June, cancer screenings had not returned to their pre-COVID-19 levels, according to data from the Epic Health Research Network. Breast, colon and cervical cancer screenings remained 29%, 36%, and 35% lower than expected, respectively.
In short, we risk a significant increase in the number of deaths and poorer outcomes from cancer if we don’t successfully address these issues during the pandemic.
Getting the story straight
Our challenge is to earn patients’ trust, so that they can safely and cost-effectively resume screening procedures for cancer.
Healthcare leaders need to explain measures they are taking to ensure a low infection risk at clinical facilities that offer screenings.
We must also assure individuals that discovery of a malignancy or a premalignant lesion can be safely treated in the clinic or hospital. Early studies show that cancer patients undergoing chemotherapy or other treatments are not at increased risk of mortality from COVID-19. Although, outcomes data is emerging from large cohort studies that will address this issue much more carefully in the next several months.
We must adhere to social distancing and mask-wearing policies in clinical facilities and communicate those policies clearly to patients and their family members. We must make such small steps as scheduling appointments and negotiating with payers as easy as possible, since every barrier to care takes on added weight during COVID-19.
It can be difficult for people to grasp the harm of not doing a procedure. But forgoing cancer screenings has the potential to derail the country’s decades-long progress in lowering cancer mortality. COVID-19 has been destructive enough. We must not let it stop measures to detect early disease—the most effective method we have to prevent deaths from cancer.
In order to understand better the impact of COVID-19 on cancer patients, the Hollings Cancer Center here at the Medical University of South Carolina (@muschollings) in Charleston joined the COVID-19 and Cancer consortium (CCC19) and is one of 120 institutions in the country collecting data on adult patients (18 and older) with cancer who have been diagnosed with COVID-19.
This is being done in order to collect and disseminate prospective, granular, uniformly organized information on cancer patients and survivors who are diagnosed with COVID-19—at scale and as rapidly as possible to understand, in real time, how this disease is affecting cancer patients.
And please don’t forget:
There are several steps we can all take to reduce our risk of getting cancer:
Don’t use tobacco in any form or expose yourself to secondhand smoke. Cancers linked to tobacco use make up to 40% of all cancers, so avoiding this exposure can have a huge benefit.
Eat a healthy diet that includes fruits and vegetables. If you choose to drink alcohol, do so in moderation, and limit intake of processed meats.
Maintain a healthy weight and stay physically active. Any amount of physical activity is helpful, but to maximize benefit, the Mayo Clinic recommends getting at least 150 minutes per week of moderate activity or 75 minutes per week of vigorous aerobic activity.
Protect yourself from exposure to the sun and avoid tanning beds or sun lamps at all costs.
Get vaccinated for hepatitis B and the human papilloma virus (HPV) at the recommended ages. Avoid risky behaviors that can lead to infections known to increase your risk of cancer, like unprotected sex or the sharing of needles used by others.
Seek routine medical care, as noted above, that includes regular self-exams and screenings for various types of cancers, such as cancer of the skin, colon, cervix and breast. These preventive exams increase your chances of discovering cancer early, when treatment is most likely to be successful.
Do not hesitate to ask your doctor about the best cancer screening schedule for you based on your medical and family history.
Remember, if we collectively, as a population, adhere to all of these recommendations, we could reduce cancer globally by as much as 40-50%—today, without any further advances in diagnostics or treatment.